ABSTRACT
Intimal sarcoma of the pulmonary artery is a rare and potentially lethal tumor, the diagnosis of which is difficult and therefore frequently delayed. The clinical signs and symptoms are nonspecific, often mimicking chronic pulmonary thromboembolism (CPTE). We report the case of a 45-year-old male under treatment for CPTE associated with pulmonary arterial hypertension and chronic cor pulmonale. There was no response to treatment with anticoagulants and sildenafil. We emphasize the difficulties in diagnosing intimal sarcoma of the pulmonary artery, the need to investigate this neoplasm in the differential diagnosis of CPTE and the systematic use of criteria for the appropriate prescription of new medications for pulmonary artery hypertension.
Keywords:
Pulmonary embolism; Hypertension, pulmonary; Hemangiosarcoma; Diagnosis, differential.
RESUMO
O sarcoma intimal de artéria pulmonar é um tumor raro e potencialmente letal, de diagnóstico difícil e, muitas vezes, tardio. Os sinais e sintomas clínicos são inespecíficos, simulando com frequência o tromboembolismo pulmonar crônico (TEPC). Apresentamos o caso de um homem de 45 anos em tratamento de TEPC associado com hipertensão arterial pulmonar e cor pulmonale crônico, sem resposta ao uso de anticoagulantes e sildenafil. Ressaltamos as dificuldades para o diagnóstico do sarcoma intimal de artéria pulmonar, a necessidade de se pesquisar essa neoplasia no diagnóstico diferencial do TEPC e a utilização sistemática de critérios para a adequada indicação dos novos medicamentos para a hipertensão arterial pulmonar.
Palavras-chave:
Embolia pulmonar; Hipertensão pulmonar; Hemangiossarcoma; Diagnóstico diferencial.
IntroductionIntimal sarcoma of the pulmonary artery is extremely rare.(1) It was first described by Mandelstamm in 1923,(2-5) and approximately two hundred cases have been reported in the literature.(4) The true incidence of intimal sarcoma of the pulmonary artery is unknown, but it is likely that this disease is underdiagnosed due to its similarity to chronic pulmonary thromboembolism (CPTE).(1,4,6) The objective of the present case report was to draw attention to the need to consider this entity in the differential diagnosis of CPTE, as well as to discuss the diagnostic methods and the therapeutic options available to treat this uncommon disease that has a dismal prognosis.
Case reportA forty-five-year-old male sought the services of Madre Teresa Hospital, located in the city of Belo Horizonte, Brazil, in order to undergo angiotomography of the chest for the follow-up treatment of recurrent pulmonary thromboembolism. The patient complained of slowly progressive dyspnea, which had started two years prior, associated with weight loss (approximately 20 kg) and occasional fever (up to 38.5°C). He reported having been through extensive assessment and having received a diagnosis of CPTE associated with pulmonary hypertension. The patient was being treated with an oral anticoagulant and had started using sildenafil (25 mg twice a day) one month prior. He reported partial improvement in his general health status with the use of those medications. In view of the degree of dyspnea-functional class III, in accordance with the World Health Organization (WHO) scale-the patient was hospitalized. The patient presented tachypnea (24 breaths/min), SaO2 of 93% on room air and at rest, tachycardia (113 bpm) and lower limb edema. Arterial pressure was 140/80 mmHg, there was turgescence of the jugular veins (4+/4), and pulmonary auscultation revealed third heart sound along the lower left sternal border and systolic ejection murmur in pulmonary focus. The liver was palpable at 4 cm from the right costal margin.
A transthoracic Doppler echocardiogram, which had been performed previously, showed moderate right heart enlargement, and pulmonary artery systolic pressure (PASP) was estimated to be 76 mmHg. A transesophageal echocardiogram demonstrated extensive thrombosis in the pulmonary artery trunk and PASP of 57 mmHg. Ultrasonography of the lower limbs revealed no signs of deep venous thrombosis. Lung perfusion scintigraphy, which was performed during hospitalization, showed low uptake in the view of the anterior and the apical-posterior segments of the left lung. The right lung was not visualized. Angiotomography of the chest revealed a large filling defect in the mediastinal and pericardial portion of the pulmonary trunk and arteries, there being enhancement of that defect after intravenous administration of contrast material (Figure 1a). In addition, there were predominantly peripheral nodules on the left (Figure 1b), as well as thickening of interlobular and peribronchovascular septa on the right, associated with upper lobe consolidation, moderate pericardial effusion and a mosaic attenuation pattern (Figure 2).
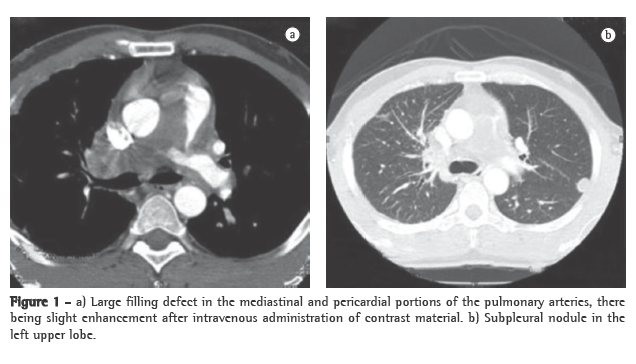
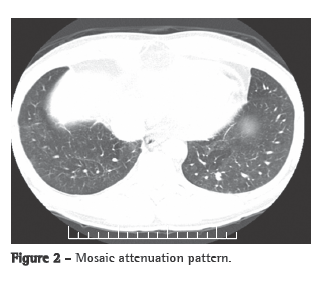
The clinical profile, together with the age of the patient, the failure of anticoagulant treatment, the tomographic alterations and the contrast enhancement, led to the hypothesis of intimal sarcoma-angiosarcoma-with pulmonary metastases. A CT-guided transthoracic biopsy of the left lung nodule was required. The specimen obtained consisted of a soft, reddish-tan filiform fragment, measuring 1.2 cm in length.
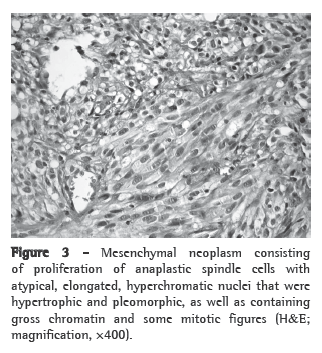
The histological sections showed a mesenchymal neoplasm consisting of proliferation of anaplastic spindle cells with atypical, elongated, hyperchromatic nuclei that were hypertrophic and pleomorphic, as well as containing gross chromatin and some mitotic figures. The cytoplasm was hardly detectable. There were rare foci of necrosis and hemorrhage (Figure 3). The lesion was well delineated in relation to the surrounding pulmonary parenchyma, which showed no relevant alterations.
Immunohistochemical analysis showed positive staining for cytokeratin AE1/AE3 only focally. All of the other markers studied (CD34, S-100, HMB-45, smooth muscle actin, desmin, CD31 and TTF-1) tested negative.
Based on the clinical, histological and immunohistochemical findings, a diagnosis of metastatic undifferentiated intimal sarcoma was made
(Figure 3).
In view of the degree of impairment resulting from the wasting syndrome, the patient was initially referred for oncological treatment prior to the surgical procedure.
After the first chemotherapy session, the patient was hospitalized again due to significant hemoptysis and subsequently died.
DiscussionIntimal sarcoma of the pulmonary artery is a quite rare(1) and highly lethal tumor(7) that affects large vessels, especially the aorta, the inferior vena cava and the pulmonary artery.(1,7) It presents as vascular obstruction due to the intraluminal growth and the associated thrombosis. Intimal sarcoma of the pulmonary artery can be confused with CPTE due to the similarity of the signs and symptoms, as well as to the progression to pulmonary hypertension(5,8,9) and the subsequent right ventricular failure associated with chronic cor pulmonale.(10) It is commonly accompanied by dyspnea, chest pain and cough.(1,6,7,9,11) Hemoptysis,(1,6,7,9,11) weight loss, fever and digital clubbing can also be found, and when present, should lead to the suspicion of intimal sarcoma of the pulmonary artery.(6,9)
The absence of deep venous thrombosis, negative results for procoagulant changes and the absence of response to anticoagulant therapy should be valued.(3) Signs of pulmonary hypertension revealed by CT,(12-14) which are common in intimal sarcoma of the pulmonary artery and in CPTE, can lead to a mistaken diagnosis of CPTE in view of its higher prevalence.(1) According to the WHO, there are three types of sarcoma of large blood vessels: angiosarcoma, leiomyosarcoma and intimal sarcoma.(7) Macroscopically, intimal sarcoma affects the tunica intima of the arteries and presents an appearance of a gelatinous or mucinous clot filling the arterial lumen. Histologically, intimal sarcoma is, for the most part, an undifferentiated or a poorly differentiated tumor consisting of spindle or epithelioid cells with marked nuclear atypia.(1)
Most cases studied immunohistochemically stain at least focally for CD34, CD31 and Fli-1, since these are markers of vascular lesions.(15) The most common histological diagnosis is malignant fibrous histiocytoma, followed by angiosarcoma, rhabdomyosarcoma and osteosarcoma. Such as in the case reported here, many intimal sarcomas are negative for most of the antibodies tested. Focal cytokeratin AE1/AE3 expression can suggest a diagnosis of metastatic sarcomatoid carcinoma. However, a diagnosis of sarcomatoid carcinoma can only be made on an immunohistochemical basis when clinical, laboratory and imaging data are associated. A diagnosis of intimal sarcoma was the most likely. We emphasize that a thorough clinical investigation, as well as a comprehensive imaging study, was performed and no other tumors were found.
Apparently, the histopathological classification does not affect the clinical approach or the prognosis of patients.(3) Intimal sarcoma of the pulmonary artery affects both genders equally,(9) with onset typically occurring in the fifth decade of life.(4,6) It is frequently diagnosed in autopsy material or in surgical pieces, which is why its true incidence is unknown. It can metastasize to the brain, the pancreas, the adrenal glands and the lungs. The prognosis is poor. Life expectancy ranges from 12 to 18 months after symptom onset,(6) and one-year and two-year survival rates are 22% and 7%, respectively.(7) Treatment includes the surgical excision of the tumor, and adjuvant radiotherapy or chemotherapy may be necessary for complementation.(1,5,11)
Judicious prescription of medications should be a constant concern among specialists, other physicians and entities involved in diagnosing, treating and caring for patients with pulmonary arterial hypertension.(16)
The case described here illustrates this problem and highlights the importance of using diagnostic and therapeutic resources properly, in accordance with the national and international guidelines currently available.
The case reported here draws attention to the need to raise the differential diagnosis in patients who are unresponsive to the current treatment of venous thromboembolism. Intimal sarcoma of the pulmonary artery is among the alternative diagnoses. Since iodinated contrast enhancement (angiotomography of the chest) can confirm the presence of the mass as well as its central location in the pulmonary trunk and arteries, which strongly suggest a diagnosis of intimal sarcoma of the pulmonary artery rather than that of CPTE, it constitutes a clue for making the former diagnosis. We emphasize the need for the proper use of the clinical methods currently available for the exact etiological definition of arterial pulmonary hypertension, prior to prescribing new medications (phosphodiesterase-5 inhibitors and inhibitors of endothelin receptors).(8,16)
References 1. Nakajima J, Morota T, Matsumoto J, Takazawa Y, Murakawa T, Fukami T, et al. Pulmonary intimal sarcoma treated by a left pneumonectomy with pulmonary arterioplasty under cardiopulmonary bypass: report of a case. Surg Today. 2007;37(6):496-9.
2. Mandelstamm M. Über primäre Neubildungen des Herzens. Virchows Arch (Pathol Anat) 1923;245:43-57.
3. Widera E, Sulica R. Pulmonary artery sarcoma misdiagnosed as chronic thromboembolic pulmonary hypertension. Mt Sinai J Med. 2005;72(6):360-4.
4. Kerr KM. Pulmonary artery sarcoma masquerading as chronic thromboembolic pulmonary hypertension. Nat Clin Pract Cardiovasc Med. 2005;2(2):108-12; quiz 113.
5. Scheffel H, Stolzmann P, Plass A, Weber A, Prêtre R, Marincek B, et al. Primary intimal pulmonary artery sarcoma: a diagnostic challenge. J Thorac Cardiovasc Surg. 2008;135(4):949-50.
6. Ozbek C, Emrecan B, Calli AO, Gurbuz A. Intimal sarcoma of the pulmonary artery with retrograde extension into the pulmonic valve and right ventricle. Tex Heart Inst J. 2007;34(1):119-21.
7. Hsing JM, Thakkar SG, Borden EC, Budd GT. Intimal pulmonary artery sarcoma presenting as dyspnea: case report. Int Semin Surg Oncol. 2007;4:14.
8. McLaughlin VV, McGoon MD. Pulmonary arterial hypertension. Circulation. 2006;114(13):1417-31.
9. Neves S, San José J, Velho HV, Oliveira M, Esteves I, Torres S, et al. Pulmonary Artery Sarcoma - diagnostic and treatment difficulties [Article in Portuguese]. Rev Port Pneumol. 2003;9(1):41-51.
10. Engelke C, Riedel M, Rummeny EJ, Marten K. Pulmonary haemangiosarcoma with main pulmonary artery thrombosis imitating subacute pulmonary embolism with infarction. Br J Radiol. 2004;77(919):623-5.
11. Parish JM, Rosenow EC 3rd, Swensen SJ, Crotty TB. Pulmonary artery sarcoma. Clinical features. Chest. 1996;110(6):1480-8.
12. Simonneau G, Galiè N, Rubin LJ, Langleben D, Seeger W, Domenighetti G, et al. Clinical classification of pulmonary hypertension. J Am Coll Cardiol. 2004;43(12 Suppl S):5S-12S.
13. Barst RJ, McGoon M, Torbicki A, Sitbon O, Krowka MJ, Olschewski H, et al. Diagnosis and differential assessment of pulmonary arterial hypertension. J Am Coll Cardiol. 2004;43(12 Suppl S):40S-47S.
14. Pietra GG, Capron F, Stewart S, Leone O, Humbert M, Robbins IM, et al. Pathologic assessment of vasculopathies in pulmonary hypertension. J Am Coll Cardiol. 2004;43(12 Suppl S):25S-32S.
15. Sebenik M, Ricci A Jr, DiPasquale B, Mody K, Pytel P, Jee KJ, et al. Undifferentiated intimal sarcoma of large systemic blood vessels: report of 14 cases with immunohistochemical profile and review of the literature. Am J Surg Pathol. 2005;29(9):1184-93.
16. Sociedade Brasileira de Pneumologia e Tisiologia. Diretrizes Brasileiras para Manejo da Hipertensão Pulmonar - 2005. J Bras Pneumol. 2005;31(2):S1-S31.
About the authors
Ana Paula Alves Valle Dornas
Physician Specializing in Pulmonology. Center for Research and Graduate Studies, Federal University of Minas Gerais School of Medical Sciences, Belo Horizonte, Brazil.
Frederico Thadeu Assis Figueiredo Campos
Coordinator. Department of Pulmonology, Madre Teresa Hospital, Belo Horizonte, Brazil.
Cláudia Juliana Rezende
Coordinator. Center for Diagnostic Imaging, Madre Teresa Hospital, Belo Horizonte, Brazil.
Carlos Alberto Ribeiro
Pathologist. Roberto Alvaranga Institute, Madre Teresa Hospital, Belo Horizonte, Brazil.
Nilson Figueiredo Amaral
Coordinator. Department of Thoracic Surgery, Madre Teresa Hospital, Belo Horizonte, Brazil.
Ricardo de Amorim Corrêa
Adjunct Professor. Department of Pulmonology, Federal University of Minas Gerais School of Medicine, Belo Horizonte, Brazil.
Study carried out in the Department of Pulmonology, Madre Teresa Hospital, in partnership with the Center for Research and Graduate Studies of the Federal University of Minas Gerais School of Medical Sciences, Belo Horizonte, Brazil.
Correspondence to: Ana Paula Alves Valle Dornas. Rua São Paulo, 2186, apto 102, Lourdes, CEP 30170-132, Belo Horizonte, MG, Brasil.
Tel 55 31 3339-8000. E-mail: anapaulaab@yahoo.com.br
Financial support: None.
Submitted: 28 November 2008. Accepted, after review: 5 March 2009.





 Read in Portuguese
Read in Portuguese
 Portuguese PDF
Portuguese PDF
 English PDF
English PDF
 Print
Print
 Send this article by email
Send this article by email
 How to cite this article
How to cite this article
 Submit a comment
Submit a comment
 Mendeley
Mendeley
 Pocket
Pocket