ABSTRACT
Objective: To develop a set of descriptive terms applied to the sensation of dyspnea (dyspnea descriptors) for use in Brazil and to investigate the usefulness of these descriptors in four distinct clinical conditions that can be accompanied by dyspnea. Methods: We collected 111 dyspnea descriptors from 67 patients and 10 health professionals. These descriptors were analyzed and reduced to 15 based on their frequency of use, similarity of meaning, and potential pathophysiological value. Those 15 descriptors were applied in 50 asthma patients, 50 COPD patients, 30 patients with heart failure, and 50 patients with class II or III obesity. The three best descriptors, as selected by the patients, were studied by cluster analysis. Potential associations between the identified clusters and the four clinical conditions were also investigated. Results: The use of this set of descriptors led to a solution with seven clusters, designated sufoco (suffocating), aperto (tight), rápido (rapid), fadiga (fatigue), abafado (stuffy), trabalho/inspiração (work/inhalation), and falta de ar (shortness of breath). Overlapping of descriptors was quite common among the patients, regardless of their clinical condition. Asthma was significantly associated with the sufoco and trabalho/inspiração clusters, whereas COPD and heart failure were associated with the sufoco, trabalho/inspiração, and falta de ar clusters. Obesity was associated only with the falta de ar cluster. Conclusions: In Brazil, patients who are accustomed to perceiving dyspnea employ various descriptors in order to describe the symptom, and these descriptors can be grouped into similar clusters. In our study sample, such clusters showed no usefulness in differentiating among the four clinical conditions evaluated.
Keywords:
Dyspnea; Pulmonary disease, chronic obstructive; Asthma; Heart failure.
RESUMO
Objetivo: Desenvolver um conjunto de termos descritores de dispneia para uso no Brasil. Investigar a utilidade desses descritores em quatro condições distintas que cursam com dispneia. Métodos: Um conjunto de 111 frases descritivas da sensação de falta de ar foi coletado a partir das informações de 67 pacientes e de 10 profissionais da saúde. Tais frases foram analisadas e reduzidas a 15 expressões, em função de sua frequência de citação, similaridade de significados e potencial importância fisiopatológica. O conjunto de expressões foi aplicado a 50 pacientes com asma, 50 com DPOC, 30 com insuficiência cardíaca e 50 com obesidade graus II ou III. Os três melhores termos selecionados pelos pacientes foram estudados por análise de agrupamentos. Também foram investigadas as possíveis associações entre os agrupamentos encontrados e as quatro condições clínicas incluídas. Resultados: O emprego dessa lista de descritores levou a uma solução com sete agrupamentos, denominados sufoco, aperto, rápido, fadiga, abafado, trabalho/inspiração e falta de ar. Houve grande superposição no uso de descritores pelos pacientes com as quatro condições clínicas. A asma mostrou associações expressivas com sufoco e trabalho/inspiração, enquanto DPOC e insuficiência cardíaca, com sufoco, trabalho/inspiração e falta de ar; e obesidade, com falta de ar apenas. Conclusões: Pacientes no Brasil habituados a sentir dispneia utilizam diferentes termos para descrever seu sintoma, e tais descrições podem ser agrupadas em conjuntos por similaridade. Tais agrupamentos não mostraram utilidade na distinção diagnóstica entre os grupos avaliados neste estudo.
Palavras-chave:
Dispneia; Doença pulmonar obstrutiva crônica; Asma; Insuficiência cardíaca.
IntroductionThe word dyspnea is derived from the Greek words dys (difficulty, bad) and pnóia (breathing), and it can be translated literally as "difficulty in breathing".(1) According to the American Thoracic Society, "dyspnea is a term used to characterize a subjective experience of breathing discomfort that consists of qualitatively distinct sensations that vary in intensity. The experience derives from interactions among multiple physiological, psychological, social, and environmental factors, and may induce secondary physiological and behavioral responses."(2) Dyspnea is certainly a major complaint in clinical practice and is the principal factor limiting the quality of life of many patients with chronic lung diseases.(3,4) Despite recent advances in the understanding of the mechanism of respiratory sensations, the large numbers of and the complexity of the interactions among receptors and neural pathways remain as obstacles to a full understanding of the mechanisms of dyspnea.(5)
There is mounting evidence that dyspnea does not involve a single, specific perception; rather, it involves a set of distinct sensations.(6-10) As has been observed for pain, different terms used by patients to describe the sensation of dyspnea might reflect the underlying pathophysiological mechanisms and therefore be related to the underlying diagnoses. For instance, in a study of healthy volunteers submitted to eight distinct respiratory stimuli, such as carbon dioxide inhalation, breathing against elastic load, and physical exercise, the authors identified clusters of descriptive terms applied to the respiratory sensations; those clusters were associated with the different agents employed.(6) In another study, involving 218 patients presenting with seven distinct cardiorespiratory conditions in the stable phase, the use of a questionnaire including 15 descriptive questions regarding their respiratory sensations revealed clusters of descriptors, the combinations of which were specific to each diagnosis.(9)
Although there have been many studies regarding the potential use of descriptive terms applied to the sensation of dyspnea (dyspnea descriptors),(11-16) there is a lack of such studies in Brazil. Cultural and linguistic differences can certainly affect the results. The objective of the present study was to develop a set of dyspnea descriptors for use in Brazil and investigate the usefulness of these descriptors in distinct clinical conditions that can be accompanied by dyspnea.
MethodsIn order to develop the descriptors, we conducted a pilot study in which 67 patients with various cardiorespiratory conditions were initially interviewed. Of those 67 patients, 25 had asthma, 20 had COPD, 17 had heart failure, and 5 had other conditions. The mean age was 45.3 years (range, 17-80 years). Of the 67 patients evaluated, 39 were female and 28 were male.
The individuals were asked how they would describe their sensation of dyspnea, and all of the information collected was noted. In that same phase, we interviewed three physicians, three nurses, and four physical therapists, all of whom suggested additional descriptors. From an extensive list including 111 descriptors (Appendix 1 ) and on the basis of the frequency of use of the terms, as well as of the similarity of meaning, we arrived at a summarized list, which comprised only 15 descriptors (Table 1). From the initial list, we also excluded descriptors that were apparently unrelated to respiratory sensations per se. The total of 15 descriptors was based on the mean number of descriptors that has been employed in international studies.


In the present study, we included patients who had been diagnosed with bronchial asthma, COPD, heart failure, or obesity (class II or III) and had been clinically stable for at least two months. The volunteers were selected from among patients under treatment at the pulmonology, cardiology, and clinical nutrition outpatient clinics of the Faculdade de Medicina de Ribeirão Preto, Universidade de São Paulo (FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine) Hospital das Clínicas, located in the city of Ribeirão Preto, Brazil. The diagnosis of asthma was established, on the basis of clinical history, physical examination, and pulmonary function test results, by residents and physicians working in the Pulmonology Department of the Hospital. The diagnosis of COPD was established on the basis of a history of exposure to smoking, symptoms consistent with the disease, and an FEV1/FVC ratio < 70%, as assessed by spirometry, even after inhaled bronchodilator use.
The patients with heart failure were diagnosed by residents and physicians working in the Cardiology Department, and the diagnosis was established on the basis of the Framingham score.(17) Patients with a body mass index (BMI) > 35 kg/m2 were included in the obesity group. We established specific exclusion criteria for each group of patients: for those diagnosed with asthma-BMI > 30 kg/m2, smoking history > 10 pack-years, and heart disease; for those diagnosed with COPD-BMI > 30 kg/m2 and heart disease; for those diagnosed with heart failure-BMI > 30 kg/m2, smoking history > 10 pack-years, and current or previous lung disease; and for those diagnosed with obesity-smoking history > 10 pack-years and current or previous heart or lung disease.
The patients were approached during an outpatient visit, and some of the patients with obesity were approached during hospitalization for dietary control. All patients were asked whether they experienced dyspnea. The questions asked included "Você sente falta de ar?" ("Do you have shortness of breath?") and "Você sente cansaço no peito para realizar esforços?" ("Do you feel fatigue of the muscles in your chest when exerting yourself physically?"). If the answer was "yes", the individual was invited to participate in the study and was asked to report to the pulmonary function laboratory in the near future. All of the patients who agreed to participate in the project gave written informed consent. The study was approved by the Human Research Ethics Committee of the FMRP-USP Hospital das Clínicas.
At the pulmonary function laboratory, all interviews of the volunteers were conducted by one of two researchers. Initially, demographic information, as well as information regarding the level of education, was obtained. Subsequently, a modification of the baseline dyspnea index developed by Mahler et al.(18) was used in order to evaluate the intensity of dyspnea during activities of daily living. The list of 15 dyspnea descriptors developed in the pilot study was then presented to the volunteers. The volunteers were instructed to indicate, by marking "Yes" or "No", whether a given descriptor applied to their sensation of dyspnea, either at rest or during intense physical activity. Subsequently, the patients were instructed to choose the 3 descriptors that best described their sensations of respiratory distress. Finally, they were instructed to choose, among the 3 descriptors previously selected, the one that provided the best description. Because there were patients who were illiterate or had difficulty in reading, the list of descriptors was read to all patients in the same manner, i.e., slowly, one by one, by one of the two researchers, in order to allow volunteers to answer all the questions confidently.
It should be highlighted that the volunteers were also asked to select, in the same manner, dyspnea descriptors from another list, obtained by translating, from English to Portuguese, sentences published in another study.(9) Because of the large volume of data, the results of that analysis will be presented in a subsequent article.
After we had obtained information related to the intensity of dyspnea and the quality of respiratory sensations, the volunteers underwent full spirometry with a Pulmonet Godard spirometer (SensorMedics, Bilthoven, The Netherlands). In addition, we collected blood samples from the brachial artery in order to perform arterial blood gas analysis with a gas analyzer (Ciba Corning 178 Gas System; Ciba Corning, Diagnostics Corp., Medfield, MA, USA). The predicted values used in order to characterize the reference values followed the equations devised by Crapo et al.(19)
For the statistical analysis, the pulmonary function test results and clinical data were expressed as means and standard deviations. The descriptors selected by the patients as being the 3 best were analyzed and grouped into domains that shared common characteristics by means of cluster analysis.(20,21) The clusters were defined in an exploratory manner in order to obtain the highest degree of similarity within a given set.
The associations between the clusters obtained and the four classes of clinical conditions analyzed were established, in an attempt to define patterns of specific sensations for each clinical situation, in accordance with the methodology employed in previously published studies.(6,9)
Initially, the number of times that the descriptors within a given cluster were chosen as the 3 best was divided by the product of the number of descriptors within that cluster and the number of patients with that specific condition. If the result was > 0.25, the cluster of descriptors was considered representative of the disease.
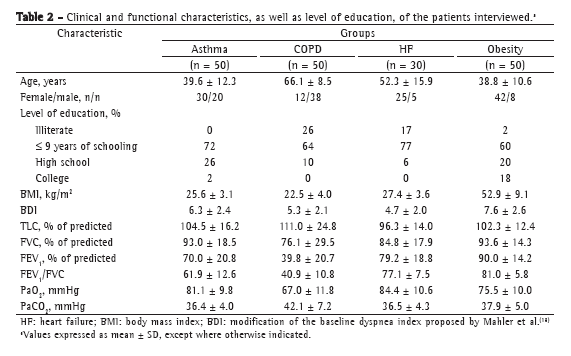
ResultsOf the 180 patients studied, 50 presented with asthma, 50 presented with COPD, 30 presented with heart failure, and 50 presented with obesity. All of the patients under study were clinically stable (Table 2). The changes in respiratory function detected were consistent with those expected for the underlying diseases (Table 2). In all of the groups, most of the interviewees reported that they had had 9 or fewer years of schooling. A substantial number of patients, principally in the COPD and heart failure groups, reported that they did not know how to read or write.
The analysis of the answers provided by the 180 volunteers allowed us to obtain seven clusters that, because of the characteristics of the descriptors involved, were designated sufoco (suffocating), aperto (tight), rápido (rapid), fadiga (fatigue), abafado (stuffy), trabalho/inspiração (work/inhalation), and falta de ar (shortness of breath), as illustrated by the dendrogram and list shown in Figure 1. The frequencies of the first three choices of descriptors, as selected by the groups of patients, are shown in Table 3. Some of the descriptors were shared by more than one group of patients.

The analysis of the associations between clusters and clinical conditions showed that the sufoco and trabalho/inspiração clusters were strongly associated with asthma, COPD, and heart failure. The last two were also significantly associated with the falta de ar cluster. Obesity was associated only with the falta de ar cluster (Table 4).
 Discussion
DiscussionWe believe that the present study is the first full study of subjective aspects of dyspnea to be published in Brazil. The results show that the use of dyspnea descriptors developed specifically for the Brazilian population allows the formation of clusters of similar descriptors, which tend to be used simultaneously. Nevertheless, the clusters used were shown to be of little use in the differential diagnosis of the four distinct clinical conditions under study.
The first studies of the language used to describe dyspnea were conducted in English.(6-9) Because of the potential influence of cultural and linguistic differences between Brazilian Portuguese and English, we made an effort to develop Brazilian Portuguese-language descriptors based on information collected from a sample of patients and health professionals working in Brazil. It is of note that many of the terms used by the patients in Brazil and selected to constitute the list of Brazilian Portuguese-language descriptors showed a correspondence with descriptors listed in previous studies as being employed by volunteers in the USA, the UK, and Mexico. Some of these descriptors included "Eu tenho a sensação que estou sufocando" and "Minha respiração fica pesada", which corresponded to the descriptors "I feel that I am smothering" and "My breathing is heavy", from studies by Mahler et al.(9) and Elliot et al.,(8) respectively, as well as to "Siento que me asfixio" and "Siento que mi respiración es pesada", from a study by Vázquez-Garcia et al.(12) This type of comparison strongly suggests that, regardless of potential regional peculiarities, the language used to describe dyspnea tends to be universal.(16)
In the present study, we attempted to investigate the use of subjective dyspnea descriptors by patients with distinct clinical conditions. Groups of volunteers with asthma, COPD, and heart failure were formed because of the high prevalence and clinical significance of these conditions. We included a group of individuals with class II or III obesity because we recognize that, in addition to its increasing prevalence, obesity is commonly accompanied by respiratory symptoms.(22,23) We made a great effort in order to guarantee that all of the patients selected to constitute the groups were specifically representative of the conditions, and the exclusion criteria attempted to limit the number of confounding factors. The means of the pulmonary function test results for the groups strongly suggest that we achieved our goal.
In the present study, we used cluster analysis for statistical exploration of the data. The method has been used in the vast majority of studies investigating clusters of dyspnea descriptors. This type of multivariate analysis is a descriptive exploratory technique, in which a cluster is defined in order to achieve the highest degree of similarity among the items that constitute it. However, one limitation of the method is that it does not strictly define the cut-off value for the construction of a cluster or determine the optimal number of clusters. Therefore, the major criterion on which to base the decision depends on the point of view and judgment of authors. This is why it is difficult to compare studies that have employed this method: the formation and number of clusters can vary from study to study.
The administration of the questionnaire comprising Brazilian Portuguese-language descriptors led to the formation of seven clusters, and the terms employed to designate those clusters attempted to translate the underlying sensation described. Because there was a certain degree of similarity among the locally developed descriptors and because of the way in which the descriptors were clustered, in comparison with results found in the international literature, the terms employed to designate some of the clusters in the present study were equivalent to the Brazilian Portuguese-language translation of terms previously employed. The sufoco, rápido, and aperto clusters represent this situation. However, the fadiga and abafado domains seem to contain attributes that are specific to the local language. In addition, there was the formation of a cluster, designated trabalho/inspiração, which contained descriptors such as "Eu faço força para o ar entrar" ("I have to struggle to get air in") and "É difícil para o ar entrar" ("It is difficult for air to get in"). The descriptor "Eu sinto falta de ar" ("I have shortness of breath") led to the formation of a single group, the meaning of which is uncertain, which is due to the generic and apparently nonspecific nature of the statement. It is of note that, in a study conducted abroad, the "work/effort" cluster included the descriptor "I feel out of breath", together with 3 other descriptors.(9)
Authors in the USA and UK have attempted to investigate relationships between the quality of respiratory sensations and the potential mechanisms that trigger distress. The sensation of "an urgent need to breathe" usually arises in the presence of increased respiratory drive triggered by hypoxemia and hypercapnia.(24) There is evidence that this type of sensation depends principally on the stimulation of central and peripheral chemoreceptors. The sensation of "effort to breathe" arises whenever the central motor command to the respiratory muscles increases.(9,10) This usually occurs in response to an increase in the respiratory muscle workload. Another condition in which this phenomenon occurs is the presence of respiratory muscle weakness due to fatigue, paralysis, or lung hyperinflation. Therefore, the sensation of "effort to breathe" is directly proportional to the ratio between the pressure generated by the respiratory muscles at a given time point and the maximum capacity of the muscles to generate pressure under the same conditions.
In studies of methacholine-induced bronchoconstriction in patients with asthma, various respiratory sensations arise in sequence.(10,25) In the presence of initial bronchoconstriction, a sensation of "chest tightness" predominates. As the FEV1 drops and the mechanical load increases, a sensation of increased "respiratory effort/work" arises. In an extremely advanced phase of bronchoconstriction, the sensation of "an urgent need to breathe" can arise, reflecting the stimulation of peripheral chemoreceptors or excessive central motor neurological command.
The distribution of the clusters that were formed, as illustrated by the dendrogram depicted in Figure 1, suggests that the sufoco and falta de ar clusters correspond to constructs that are greatly independent, although their pathophysiological correspondence is uncertain. It is possible that sufoco is somehow related to the sensation of "an urgent need to breathe". In contrast, falta de ar seems to be such a nonspecific descriptor that the sensation can be the result of the sum of numerous simultaneous pathophysiological changes. On the basis of the data available in the literature, the aperto cluster might reflect bronchospasm. However, the aperto cluster showed no association with the presence of asthma, which is evidence against this possibility. The rápido cluster shared a root with the aperto cluster, suggesting that the two sensations might be related. It is possible that the fadiga cluster is related to an increase in respiratory muscle work. Because of its proximity with the fadiga cluster, the abafado cluster might also be related, at least in part, to phenomena of that nature. Although other authors have found a "work/effort" cluster, the only study in which the "inhalation" cluster was well defined was the study conducted by Mahler et al. in 1996.(9) The trabalho/inspiração cluster found in the present study might reflect respiratory muscle overload associated with difficulty in inhaling.
In the present study, we also attempted to establish associations between the clusters obtained and the four types of conditions analyzed. Asthma was significantly associated with the sufoco and trabalho/inspiração clusters, whereas COPD and heart failure were associated with the sufoco, trabalho/inspiração, and falta de ar clusters. Obesity was associated only with the falta de ar cluster. Overlapping of descriptors was therefore quite common among the patients, regardless of their clinical condition, and the use of such descriptors was not useful in differentiating among the conditions, which is in disagreement with what has been proposed by various authors. However, our results are in agreement with those of certain other studies, which reported that the use of dyspnea descriptors is not sufficiently specific for differential diagnoses, because they reflect sensations that are shared by a variety of conditions.(26-28)
The present study has a series of limitations, among which are the small number of conditions evaluated (only four) and the fact that the choices of dyspnea descriptors by the volunteers were based exclusively on their memory. Had the interview regarding the perception of the symptom been conducted immediately after a dyspnea-inducing stimulus, such as running on a treadmill, the results might have been different. In addition, the set of descriptors employed in the present study was developed on the basis of the answers provided by patients living in a rural town in southeastern Brazil. Because of the immensity of the Brazilian territory and the enormous cultural diversity of the country, it is very likely that individuals living in other regions would use other terms to designate the sensation of shortness of breath. It should also be highlighted that the level of education of the patients treated at our hospital, including the volunteers evaluated in the present study, was not high. Therefore, intellectual limitations in terms of verbalizing the sensations and understanding the terms employed might also have had a negative impact on the reliability of the results. Therefore, the set of descriptors listed in the present study and the result of its application do not automatically apply to all patients with dyspnea in Brazil.
The results of the present study allow us to conclude that, in Brazil, patients who habitually experience dyspnea use a variety of terms to describe their symptoms and that such descriptions can be grouped into similar clusters. Although such clusters of descriptors can theoretically reflect the underlying mechanisms of dyspnea, they showed no usefulness in differentiating among the four clinical conditions evaluated in the present study. Additional investigations are needed in order to clarify whether the word "dyspnea" actually refers to various distinct sensations or whether patients refer to the same sensation using various descriptors.
References1. Curley FJ. Dyspnea. In: Irwin RS, Curley FJ, Grossman RF. Diagnosis and Treatment of Symptoms of the Respiratory Tract. Armonk: Futura Pub Co,; 1997.
2. Dyspnea. Mechanisms, assessment, and management: a consensus statement. American Thoracic Society. Am J Respir Crit Care Med. 1999;159(1):321-40.
3. Martinez TY, Pereira CA, dos Santos ML, Ciconelli RM, Guimarães SM, Martinez JA. Evaluation of the short-form 36-item questionnaire to measure health-related quality of life in patients with idiopathic pulmonary fibrosis. Chest. 2000;117(6):1627-32.
4. Katsura H, Yamada K, Wakabayashi R, Kida K. The impact of dyspnoea and leg fatigue during exercise on health-related quality of life in patients with COPD. Respirology. 2005;10(4):485-90.
5. Burki NK, Lee LY. Mechanisms of dyspnea. Chest. 2010;138(5):1196-201.
6. Simon PM, Schwartzstein RM, Weiss JW, Lahive K, Fencl V, Teghtsoonian M, et al. Distinguishable sensations of breathlessness induced in normal volunteers. Am Rev Respir Dis. 1989;140(4):1021-7.
7. Simon PM, Schwartzstein RM, Weiss JW, Fencl V, Teghtsoonian M, Weinberger SE. Distinguishable types of dyspnea in patients with shortness of breath. Am Rev Respir Dis. 1990;142(5):1009-14.
8. Elliott MW, Adams L, Cockcroft A, MacRae KD, Murphy K, Guz A. The language of breathlessness. Use of verbal descriptors by patients with cardiopulmonary disease. Am Rev Respir Dis. 1991;144(4):826-32.
9. Mahler DA, Harver A, Lentine T, Scott JA, Beck K, Schwartzstein RM. Descriptors of breathlessness in cardiorespiratory diseases. Am J Respir Crit Care Med. 1996;154(5):1357-63.
10. Manning HL, Schwartzstein RM. Pathophysiology of dyspnea. N Engl J Med. 1995;333(23):1547-53.
11. Wilcock A, Crosby V, Hughes A, Fielding K, Corcoran R, Tattersfield AE. Descriptors of breathlessness in patients with cancer and other cardiorespiratory diseases. J Pain Symptom Manage. 2002;23(3):182-9.
12. Vázquez-García JC, Balcázar-Cruz CA, Cervantes-Méndez G, Mejía-Alfaro R, Cossío-Alcántara J, Ramírez-Venegas A. Descriptors of breathlessness in Mexican Spanish [Article in Spanish]. Arch Bronconeumol. 2006;42(5):211-7.
13. Caroci Ade S, Lareau SC. Descriptors of dyspnea by patients with chronic obstructive pulmonary disease versus congestive heart failure. Heart Lung. 2004;33(2):102-10.
14. Hardie GE, Janson S, Gold WM, Carrieri-Kohlman V, Boushey HA. Ethnic differences: word descriptors used by African-American and white asthma patients during induced bronchoconstriction. Chest. 2000;117(4):935-43.
15. Harver A, Mahler DA, Schwartzstein RM, Baird JC. Descriptors of breathlessness in healthy individuals: distinct and separable constructs. Chest. 2000;118(3):679-90.
16. Mahler DA, Harver A. Do you speak the language of dyspnea? Chest. 2000;117(4):928-9.
17. McKee PA, Castelli WP, McNamara PM, Kannel WB. The natural history of congestive heart failure: the Framingham study. N Engl J Med. 1971;285(26):1441-6.
18. Stoller JK, Ferranti R, Feinstein AR. Further specification and evaluation of a new clinical index for dyspnea. Am Rev Respir Dis. 1986;134(6):1129-34.
19. Crapo RO, Morris AH, Clayton PD, Nixon CR. Lung volumes in healthy nonsmoking adults. Bull Eur Physiopathol Respir. 1982;18(3):419-25.
20. Dawson-Saunders B, Trapp RG. Basic and Clinical Biostatistics. Norwalk (CT): Appleton & Lange; 1990.
21. Frei F. Análise de agrupamentos: Estudo metodológico e aplicações em epidemiologia [dissertation]. São Paulo: Universidade de São Paulo; 1998.
22. Sahebjami H. Dyspnea in obese healthy men. Chest. 1998;114(5):1373-7.
23. Teixeira CA, Dos Santos JE, Silva GA, de Souza ES, Martinez
JA. Prevalence of and the potential physiopathological mechanisms involved in dyspnea in individuals with class II or III obesity. J Bras Pneumol. 2007;33(1):28-35.
24. Banzett RB, Lansing RW, Reid MB, Adams L, Brown R. 'Air hunger' arising from increased PCO2 in mechanically ventilated quadriplegics. Respir Physiol. 1989;76(1):53-67.
25. Binks AP, Moosavi SH, Banzett RB, Schwartzstein RM. "Tightness" sensation of asthma does not arise from the work of breathing. Am J Respir Crit Care Med. 2002;165(1):78-82.
26. Wilcock A, Crosby V, Hughes A, Fielding K, Corcoran R, Tattersfield AE. Descriptors of breathlessness in patients with cancer and other cardiorespiratory diseases. J Pain Symptom Manage. 2002;23(3):182-9.
27. Garrard A, Williams M. The language of dyspnea: a systematic review. Int J Appl Health Sci Pract. 2008;6(1):1540-80.
28. Smith J, Albert P, Bertella E, Lester J, Jack S, Calverley P. Qualitative aspects of breathlessness in health and disease. Thorax. 2009;64(8):713-8.
Study carried out in the Pulmonology Section of the Department of Clinical Medicine, Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Ribeirão Preto, Brazil.
Correspondence to: José Antônio Baddini Martinez. Avenida Bandeirantes, 3900, CEP 14048-900, Ribeirão Preto, SP, Brasil.
Tel. 55 16 3602-2531. E-mail: baddini@fmrp.usp.br
Financial support: None.
Submitted: 28 March 2011. Accepted, after review: 9 May 2011.
About the authorsChristiane Aires Teixeira
Pulmonologist. Brasília, Brazil.
Antonio Luiz Rodrigues Júnior
Associate Professor. Department of Social Medicine. Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Ribeirão Preto, Brazil.
Luciana Cristina Straccia
Biomedical Professional. Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Hospital das Clínicas, Ribeirão Preto, Brazil.
Élcio dos Santos Oliveira Vianna
Associate Professor. Department of Clinical Medicine, Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Ribeirão Preto, Brazil.
Geruza Alves da Silva
Associate Professor. Department of Clinical Medicine, Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Ribeirão Preto, Brazil.
José Antônio Baddini Martinez
Associate Professor. Department of Clinical Medicine, Faculdade de Medicina de Ribeirão Preto da Universidade de São Paulo - FMRP-USP, University of São Paulo at Ribeirão Preto School of Medicine - Ribeirão Preto, Brazil.






