ABSTRACT
Objective: There is evidence that asthma is associated with an increase in psychiatric symptoms and mental disorders. This association can make it difficult to achieve asthma control. The purpose of this study was to determine whether the level of asthma control is associated with anxiety and depression. Methods: A cross-sectional study involving 78 patients with confirmed moderate or severe asthma and under regular treatment at the Asthma Outpatient Clinic of the Federal University of São Paulo Hospital São Paulo, in the city of São Paulo, Brazil. The patients were divided into two groups by asthma control status, as assessed by the asthma control test, and were subsequently compared in terms of demographic, clinical, and spirometric data, as well as scores for asthma quality of life and hospital anxiety/depression. Results: The sample was predominantly female. Of the 78 patients, 49 (63%) were classified as having uncontrolled asthma. The prevalence of anxiety and of anxiety+depression was significantly higher among patients with uncontrolled asthma than among those with controlled asthma (78% and 100%; p = 0.04 and p = 0.02, respectively), whereas there were no differences between the two groups in terms of the prevalence of depression, spirometry results, or quality of life score. Conclusions: In this sample, the prevalence of anxiety symptoms was higher in the patients with uncontrolled asthma than in those with controlled asthma.In the evaluation of asthma patients, the negative impact of mood states ought to be taken into consideration when asthma control strategies are being outlined.
Keywords:
Asthma; Anxiety; Depression; Cross-sectional studies.
RESUMO
Objetivo: Existem evidências da associação entre asma e sintomas psiquiátricos e transtornos mentais. Essa associação pode resultar em dificuldades de se atingir o controle da asma. O objetivo deste estudo foi avaliar a associação de ansiedade e depressão com o controle da asma. Métodos: Estudo transversal com 78 pacientes asmáticos com diagnóstico confirmado de asma moderada a grave e regularmente tratados no Ambulatório de Asma do Hospital São Paulo da Universidade Federal de São Paulo, São Paulo (SP). Os pacientes foram divididos em dois grupos em relação ao status de controle de asma, determinado através do teste de controle da asma, e, posteriormente, comparados em termos de dados demográficos, clínicos e espirométricos, escore do questionário de qualidade de vida para asma e escore da escala hospitalar de ansiedade e depressão. Resultados: A maioria era do sexo feminino. Dos 78 pacientes, 49 (63%) foram classificados como tendo asma não controlada. A prevalência de ansiedade e do binômio ansiedade/depressão foi significantemente maior entre os pacientes não controlados do que nos controlados (78% e 100%; p = 0,04 e p = 0,02, respectivamente), enquanto nem prevalência de depressão, nem os dados espirométricos ou de qualidade de vida diferiram entre os grupos. Conclusões: Nesta amostra, os pacientes com asma não controlada apresentaram uma maior prevalência de sintomas de ansiedade que aqueles com asma controlada. Na avaliação de pacientes asmáticos, deve-se considerar o impacto negativo dos distúrbios de humor nas estratégias de controle da asma.
Palavras-chave:
Asma; Ansiedade; Depressão; Estudos transversais.
IntroductionWorldwide, asthma is one of the most common chronic diseases. The concept of asthma control was clearly outlined in the most recent revision of the Global Initiative for Asthma (GINA) guidelines. This concept encompasses asthma severity, asthma education, and management of the pharmacological treatment based on a step-up or step-down approach. Access to effective treatment allows asthma to be well controlled in most patients.(1,2) When uncontrolled, asthma can severely limit activities of daily living and can be even fatal.(1) Although impressive efforts have been made in order to improve asthma care over the last decade, asthma continues to be poorly controlled in a considerable
number of patients.(1-3)
The asthma control test (ACT) is one of the tools that have been developed to quantify asthma control status. The ACT was designed to assess the multidimensional nature of asthma.(4) Many factors contribute to the lack of adequate control. One such factor, psychiatric disorders, has been studied as a modulator of uncontrolled asthma.(5-8)
Psychiatric disorders, mostly anxiety and depression, have been associated with asthma.(9-13) Asthma patients and patients with anxiety both exhibit a defensive behavior; the former, because of their repressive style of coping, might have an impaired ability to perceive asthma symptoms, a necessary prerequisite for following a personal asthma action plan, and the latter might have a heightened perception of their symptoms.(6,14) Therefore, the presence of anxiety or depression could affect the results of a self-administered multidimensional questionnaire such as the ACT.
Because of the abovementioned considerations, the objective of the present study was to determine whether asthma control status, as assessed by the ACT, is associated with anxiety and depression in patients under regular treatment for moderate or severe asthma.
MethodsThis was a cross-sectional study conducted at the Asthma Outpatient Clinic of the Federal University of São Paulo Hospital São Paulo, a tertiary-care facility located in the city of São Paulo, Brazil. This clinic has a tailored program for asthma patients that consists of asthma education and pharmacological therapy, in accordance with the 2006 GINA guidelines.(1)
The study protocol was approved by the local research ethics committee (ruling no. 1375/06), and all participants gave written informed consent.
The inclusion criteria were having a confirmed diagnosis of moderate or severe asthma,(1) being 18 years of age, and having been under outpatient follow-up treatment for more than six months.(15)
We selected 82 patients, 4 of whom were excluded: 2 because they declined to participate; and 2 because there were missing data. Therefore, 78 patients completed the study.
We collected demographic data (age and gender), clinical data (maintenance medication in use for over a month), and spirometric data (FEV1, FVC, and FEV1/FVC ratio prior to and after the use of an inhaled short-acting 2 agonist). Spirometry was performed in accordance with the Brazilian Thoracic Society guidelines.(16) The patients also completed the following instruments: the ACT; the asthma quality of life questionnaire (ACQL); and the hospital anxiety and depression scale (HADS).
The level of asthma control was assessed with the ACT,(4) a self-administered questionnaire that is useful for quantifying asthma control and has been validated for such use. This questionnaire was developed in order to assess asthma control, and it has shown strong evaluative and discriminative properties.(4) It consists of 5 questions, related to the four weeks preceding the evaluation, addressing multiple dimensions of control, including episodes of breathlessness, nocturnal awakenings, limitations in activities of daily living, self-rating of asthma control, and need for relief medication. Each question is scored on a 6-point scale-from 0 (good control) to 5 (poor control)-and the total score therefore ranges from 5 to 25. A score 20 on the ACT is defined as controlled asthma.
Asthma severity was stratified into five levels in accordance with 2006 GINA guidelines(1): level 1, use of relief medications only; level 2, use of low doses of inhaled glucocorticosteroids (200-400 µg/day of budesonide); level 3: use of medium doses of inhaled glucocorticosteroids (400-800 µg/day of budesonide); level 4, use of inhaled glucocorticosteroids and a long-acting inhaled 2 agonist or montelukast/theophylline; and level 5, use of high doses of inhaled glucocorticosteroids plus a long-acting inhaled 2 agonist plus a third medication or an oral corticosteroid.
The AQLQ is a disease-specific instrument for the determination of quality of life that has been validated for use in clinical trials. It contains 32 questions comprising four domains: activity limitation, symptoms, emotional function, and environmental stimuli. Each item is scored on a 7-point scale, on which 1 indicates severe impairment, and 7 indicates no impairment.(17)
Anxiety and depression were assessed with the Portuguese-language version of the HADS, which has been extensively used in screening for psychiatric morbidity.(18) It consists of 14 questions-7 for anxiety and 7 for depression, each scored from 0 to 3, the maximum score for either therefore being 21. Higher scores indicate more symptoms. A HADS anxiety score of 8 was considered diagnostic of anxiety, whereas a HADS depression score of 9 was considered diagnostic of depression.(19,20)
Statistical analysisThe results are expressed as means and standard deviations or as medians and interquartile ranges. Categorical variables were compared using the chi-square test or Fisher's exact test. Depending on the distribution, continuous variables were compared by the unpaired t-test or Mann-Whitney test. Values of p < 0.05 were considered statistically significant. Statistical analyses were performed using the statistical freeware R, version 2.10.1 (R Development Core Team, 2009).
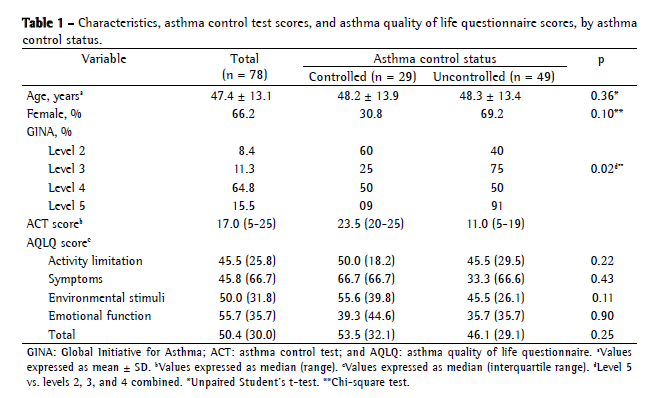
ResultsAs expected, females accounted for the vast majority (66%) of our sample, although there was no statistically significant difference between the genders in terms of asthma control status. Approximately 60% of the patients had uncontrolled asthma according to their ACT scores (< 20).
Uncontrolled asthma was significantly more common in the patients in whom asthma severity was classified as level 5 than in those in whom it was classified as level 2, 3, or 4, even when the last three were combined.
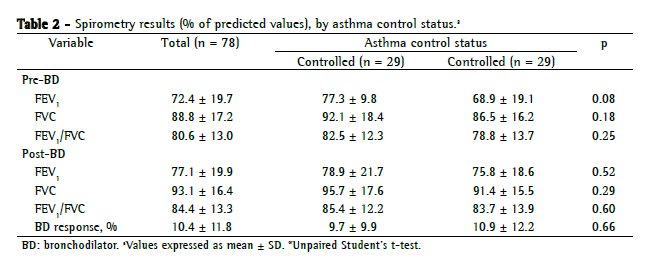
The quality of life scores did not differ between the patients with controlled asthma and those with uncontrolled asthma (Table 1). In addition, the pre- and post-bronchodilator spirometric values did not differ between the controlled asthma and uncontrolled asthma groups (Table 2).
We found that HADS scores diagnostic of anxiety, as well as those diagnostic of anxiety+depression, were significantly associated with uncontrolled asthma (Table 3). The prevalence of psychiatric disorders was significantly higher among the patients with uncontrolled asthma (Figure 1).


Figure 2 shows the distribution of the patients with psychiatric disorders (HADS scores diagnostic of anxiety, depression, or anxiety+depression), by ACT score.
 Discussion
DiscussionOf the patients evaluated in this study, 53% had anxiety, depression, or anxiety+depression. This is in accordance with the findings of various studies showing that the prevalence of anxiety and depressive disorders is elevated among asthma patients.(9,21,22)
In our study, the overwhelming majority of the patients not only exhibited the anxiety profile but also had uncontrolled asthma. In addition, none of the patients with controlled asthma, according to the ACT, had anxiety+depression. It has been reported that there is a strong association between psychiatric disorders and uncontrolled asthma.(9,10,23) Might this association be two sides of the same coin? On the one hand, the higher prevalence of anxiety among patients with uncontrolled asthma might promote mood disorders, which in turn might increase symptom perception in such patients, thereby reducing their perception of asthma control.(9,14) On the other hand, the respiratory symptoms that are secondary to mood disorders might impede the evaluation of asthma control, because certain symptoms of anxiety (shortness of breath and rapid HR) and depression (insomnia and fatigue) could overlap with those of asthma. To avoid this potential bias, we used the HADS, which is widely used in hospital outpatient settings and has been validated as a screening tool for anxiety and depressive illness.(12,20) Clinical data, such as spirometry results, as well as data related to use of medication and to quality of life, were also collected in order to improve the description of the asthma status associated with a given psychiatric profile.
Asthma is a chronic inflammatory disease whose main characteristic is a huge variability in its clinical expression. Even when disease control is achieved, all asthma patients have to deal with two major features: the risk of future exacerbations; and the decrease in pulmonary function. These features might lead to an ongoing stress situation. It has been hypothesized that chronic psychological stress causes a chronic pro-inflammatory state.(24) Evidence to support this conjecture comes from two studies, which showed that stress is associated with increased leukocyte production of pro-inflammatory superoxides and cytokines.(25,26)
There is a close relationship between the difficulty in achieving asthma control and psychiatric disease. A multidimensional, integrative approach to health care should be considered when assessing patients with asthma.(23) Physicians should be aware of the fact that anxiety and depressive disorders increase the risk of poor adherence to appropriate
asthma management regimens.
Although the relationships between disease severity and psychological distress are well documented, we still understand little about whether the disease causes distress, or whether distress in some way undermines disease control.(6) Other studies have shown that psychologically distressed patients tend to report worse illness even when objective measures do not bear that out.(27) This could explain the fact that, in the present study, in which the level of asthma control was determined with a self-report questionnaire, spirometry results, and quality of life scores did not differ significantly between the "controlled" and "uncontrolled" groups.
In the population studied, we found no significant differences between the patients with uncontrolled asthma and those with controlled asthma in
terms of demographic data, spirometry results, or quality of life score.
Despite the fact that females accounted for the majority of our study sample, they were proportionally distributed by asthma control status. Nor did anxiety and depression scores differ between the genders, although anxiety and insomnia have been reported to be more common among women with asthma than among men with asthma.(28) It is crucial to consider the differential impact of negative mood states when assessing asthma control and quality of life.(24)
The present study has the intrinsic limitations of a cross-sectional observational study. Therefore, it is impossible to determine whether anxiety was the cause or the consequence of uncontrolled asthma.
Another potential limitation is the fact that, in order to avoid the bias of including undertreated patients, which would have increased the number of patients with uncontrolled asthma, we only included patients participating in a special education program, on an intention-to-treat basis.
In conclusion, the prevalence of anxiety was higher in the patients with uncontrolled asthma than in those with controlled asthma. It is noteworthy that, in the evaluation of asthma patients, the negative impact that mood states have on asthma control ought to be taken into consideration.
References1. Global Initiative for Asthma. Global Strategy for Asthma Management and Prevention. NIH publication, no. 02-3659. Bethesda: National Institutes of Health; National Heart, Lung, and Blood Institute; 2006.
2. Bateman ED, Boushey HA, Bousquet J, Busse WW, Clark TJ, Pauwels RA, et al. Can guideline-defined asthma control be achieved? The Gaining Optimal Asthma ControL study. Am J Respir Crit Care Med. 2004;170(8):836-44.
3. Barnes PJ, Jonsson B, Klim JB. The costs of asthma. Eur Respir J. 1996;9(4):636-42.
4. Nathan RA, Sorkness CA, Kosinski M, Schatz M, Li JT, Marcus P, et al. Development of the asthma control test: a survey for assessing asthma control. J Allergy Clin Immunol. 2004;113(1):59-65.
5. Chung KF, Godard P, Adelroth E, Ayres J, Barnes N, Barnes P, et al. Difficult/therapy-resistant asthma: the need for an integrated approach to define clinical phenotypes, evaluate risk factors, understand pathophysiology and find novel therapies. ERS Task Force on Difficult/Therapy-Resistant Asthma. European Respiratory Society. Eur Respir J. 1999;13(5):1198-208.
6. Centanni S, Di Marco F, Castagna F, Boveri B, Casanova F, Piazzini A. Psychological issues in the treatment of asthmatic patients. Respir Med. 2000;94(8):742-9.
7. Goodwin RD, Eaton WW. Asthma and the risk of panic attacks among adults in the community. Psychol Med. 2003;33(5):879-85.
8. Goodwin RD, Jacobi F, Thefeld W. Mental disorders and asthma in the community. Arch Gen Psychiatry. 2003;60(11):1125-30.
9. Di Marco F, Verga M, Santus P, Giovannelli F, Busatto P, Neri M, et al. Close correlation between anxiety, depression, and asthma control. Respir Med. 2010;104(1):22-8.
10. Lavoie KL, Cartier A, Labrecque M, Bacon SL, Lemière C, Malo JL, et al. Are psychiatric disorders associated with worse asthma control and quality of life in asthma patients? Respir Med. 2005;99(10):1249-57.
11. Kullowatz A, Kanniess F, Dahme B, Magnussen H, Ritz T. Association of depression and anxiety with health care use and quality of life in asthma patients. Respir Med. 2007;101(3):638-44.
12. Heaney LG, Conway E, Kelly C, Gamble J. Prevalence of psychiatric morbidity in a difficult asthma population: relationship to asthma outcome. Respir Med. 2005;99(9):1152-9.
13. Oraka E, King ME, Callahan DB. Asthma and serious psychological distress: prevalence and risk factors among US adults, 2001-2007. Chest. 2010;137(3):609-16.
14. Kuehn BM. Asthma linked to psychiatric disorders. JAMA. 2008;299(2):158-60.
15. de Oliveira MA, Faresin SM, Bruno VF, de Bittencourt AR, Fernandes AL. Evaluation of an educational programme for socially deprived asthma patients. Eur Respir J. 1999;14(4):908-14.
16. Pereira C. Espirometria. J Pneumol. 2002;28(Suppl 3):S1-S82.
17. Oliveira MA, Fernandes AL, Santos LA, Carvalho MA, Faresin SM, Santoro IL. Discriminative aspects of SF-36 and QQL-EPM related to asthma control. J Asthma. 2007;44(5):407-10.
18. Nishimura K, Hajiro T, Oga T, Tsukino M, Ikeda A. Health-related quality of life in stable asthma: what are remaining quality of life problems in patients with well-controlled asthma? J Asthma. 2004;41(1):57-65.
19. Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67(6):361-70.
20. Botega NJ, Bio MR, Zomignani MA, Garcia C Jr, Pereira WA. Mood disorders among inpatients in ambulatory and validation of the anxiety and depression scale HAD [Article in Portuguese]. Rev Saude Publica. 1995;29(5):355-63.
21. Katon WJ, Richardson L, Russo J, Lozano P, McCauley E. Quality of mental health care for youth with asthma and comorbid anxiety and depression. Med Care. 2006;44(12):1064-72.
22. Cooper CL, Parry GD, Saul C, Morice AH, Hutchcroft BJ, Moore J, et al. Anxiety and panic fear in adults with asthma: prevalence in primary care. BMC Fam Pract. 2007;8:62.
23. Strine TW, Mokdad AH, Balluz LS, Berry JT, Gonzalez O. Impact of depression and anxiety on quality of life, health behaviors, and asthma control among adults in the United States with asthma, 2006. J Asthma. 2008;45(2):123-33.
24. Lavoie KL, Bacon SL, Barone S, Cartier A, Ditto B, Labrecque M. What is worse for asthma control and quality of life: depressive disorders, anxiety disorders, or both? Chest. 2006;130(4):1039-47.
25. Kang DH, Coe CL, McCarthy DO. Academic examinations significantly impact immune responses, but not lung function, in healthy and well-managed asthmatic adolescents. Brain Behav Immun. 1996;10(2):164-81.
26. Kang DH, Coe CL, McCarthy DO, Ershler WB. Immune responses to final exams in healthy and asthmatic adolescents. Nurs Res. 1997;46(1):12-9.
27. Goldney RD, Ruffin R, Fisher LJ, Wilson DH. Asthma symptoms associated with depression and lower quality of life: a population survey. Med J Aust. 2003;178(9):437-41.
28. Sundberg R, Torén K, Franklin KA, Gislason T, Omenaas E, Svanes C, et al. Asthma in men and women: treatment adherence, anxiety, and quality of sleep. Respir Med. 2010;104(3):337-44.
*Study carried out in the Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of
São Paulo/Paulista School of Medicine - São Paulo, Brazil.
Correspondence to: Ana Luisa Godoy Fernandes. Disciplina de Pneumologia, Rua Botucatu, 740, 3° andar, CEP 04023-004, São Paulo, SP, Brasil.
Tel 55 11 5549-1830. Fax: 55 11 5904-2897. E-mail: analuisa@pneumo.epm.br
Financial support: None.
Submitted: 11 March 2010. Accepted, after review: 1 September 2010.
**A versão completa em português deste artigo está disponível em www.jornaldepneumologia.com.br
About the authorsAline Arlindo Vieira
Medical Student. Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of São Paulo/Paulista School of Medicine - São Paulo, Brazil.
Ilka Lopes Santoro
Associate Professor of Pulmonology. Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of São Paulo/Paulista School of Medicine - São Paulo, Brazil.
Samir Dracoulakis
Doctoral Student. Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of São Paulo/Paulista School of Medicine - São Paulo, Brazil.
Lilian Ballini Caetano
Physician. Department of Pulmonology, Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of São Paulo/Paulista School of Medicine - São Paulo, Brazil.
Ana Luisa Godoy Fernandes
Tenured Associate Professor. Department of Pulmonology, Universidade Federal de São Paulo/Escola Paulista de Medicina - UNIFESP/EPM, Federal University of São Paulo/Paulista School of Medicine - São Paulo, Brazil.






