ABSTRACT
Objective: To investigate the symptoms most frequently found in children with a polysomnographic diagnosis of obstructive sleep apneahypopnea
syndrome (OSAHS). Methods: We evaluated 38 children consecutively referred to the sleep laboratory with suspicion of OSAHS
between June of 2003 and December of 2004. The patients were submitted to a pre-sleep questionnaire and to polysomnography. Results: The
mean age was 7.8 ± 4 years (range, 2-15 years), and 50% of the children were male. Children without apnea accounted for 7.9% of the
sample. The obstructive sleep apnea observed in the remainder was mild in 42.1%, moderate in 28.9% and severe in 22.1%. Severe cases of
apnea were most common among children under the age of six (pre-school age). In children with OSAHS, the most common symptoms were
snoring and nasal obstruction, which were observed in 74.3 and 72.7% of the children, respectively. Excessive sleepiness and bruxism were
seen in 29.4 and 34.3%, respectively, and reflux disease was seen in only 3.1%. Restless legs and difficulty in falling asleep were identified
in 65 and 33%, respectively. All of the children diagnosed with severe OSAHS also presented snoring and bruxism. Conclusions: Snoring
and nasal obstruction were the most common symptoms found in our sample of children and adolescents with OSAHS. In addition, OSAHS
severity was associated with being in the lower age bracket.
Keywords:
Obstructive sleep apnea; Polysomnography; Pediatrics; Snoring.
RESUMO
Objetivos: Investigar os sintomas mais freqüentes encontrados em crianças com diagnóstico polissonográfico de síndrome da apnéiahipopnéia
obstrutiva do sono (SAHOS). Métodos: Foram avaliadas 38 crianças consecutivamente encaminhadas ao laboratório do sono
com suspeita de SAHOS no período de junho de 2003 a dezembro de 2004. Os pacientes foram submetidos a um questionário pré-sono e
a polissonografia. Resultados: A idade média foi de 7,8 ± 4 anos (variação, 2-15 anos), sendo 50% das crianças do sexo masculino. Não
apnéicos corresponderam a 7,9% dos pesquisados, distúrbio leve obstrutivo do sono ocorreu em 42,1%, moderado em 28,9% e severo em
22,1%. Observou-se maior freqüência de casos severos de apnéia entre crianças menores de seis anos (idade pré-escolar). Dentre as crianças
com SAHOS, os sintomas mais citados foram ronco e obstrução nasal, presentes em 74,3 e 72,7% das crianças, respectivamente. Sonolência
excessiva e bruxismo ocorreram em, respectivamente, 29,4 e 34,3% dos casos e doença do refluxo em apenas 3,1%. Agitação das pernas e
dificuldade para iniciar o sono foram encontradas em, respectivamente, 65 e 33% dos avaliados. Todas as crianças que apresentaram SAHOS
de grau severo tinham queixa de ronco e bruxismo. Conclusões: Nossos resultados mostraram que os sintomas mais freqüentes em crianças
e adolescentes com SAHOS são ronco e obstrução nasal. Além disso, quadros mais graves da SAHOS estão associados à menor faixa etária.
Palavras-chave:
Apnéia obstrutiva do sono; Polissonografia; Pediatria; Ronco.
IntroductionThe obstructive sleep apnea-hypopnea syndrome (OSAHS) is an intrinsic sleep disturbance characterized by repeated episodes of partial or complete obstruction of the upper airways resulting in oxygen (oxygen-hemoglobin) desaturation and alterations in the sleep architecture.(1) The symptoms of this syndrome in children were first described by William Osler in 1892.(2) However, due to an increase in its incidence in the last decades, it has now received greater attention from the scientific community. This increase in incidence is due, principally, to the advent of polysomnography, which provides a more accurate and earlier diagnosis, as well as to the decrease in the number of tonsillectomies.(3)
The principal symptoms of OSAHS are snoring, forced mouth breathing, intense movement during sleep, nocturnal enuresis and night sweats, together with cognitive and behavioral alterations such as attention deficit and hyperactivity; which can compromise learning and cause underachievement in school.(4) Having OSAHS can also lead to growth delay and occasionally to cardiorespiratory complications such as pulmonary hypertension and cor pulmonale. This syndrome has a multifactorial etiology involving structural, obstructive and neuromotor factors. However, most cases in children are secondary to adenoid and tonsil hypertrophy. Other causes include obesity, craniofacial malformation and neuromuscular diseases.(5)
It is estimated that the prevalence of snoring in children is 3-12%, and that that of OSAHS is 0.7-3%.(1) Although it can occur at any age, from birth to adolescence, OSAHS predominantly affects preschoolers, in whom hypertrophy of the lymphoid tissue in the upper airways is more common. The differential diagnosis must include central apnea and primary snoring. Polysomnography can make this differentiation. It is considerer the method of choice to confirm the diagnosis of OSAHS, evaluate the severity of the disease and calculate the risk of postoperative complications.(6)
The prognosis and the long-term evolution of children with this syndrome have not yet been studied in depth. Most children present complete resolution of the symptoms after tonsillectomy is performed.(7) Other therapeutic options are the use of continuous positive airway pressure and other surgical procedures specifically indicated in children with craniofacial abnormalities.(3,5)
The worldwide increase in the prevalence of obesity, attention deficit disorder and hyperactivity in children makes OSAHS an emergent public health problem. The objective of this study was to investigate the symptoms most frequently found in children with polysomnographic diagnosis of OSAHS.
MethodsWe evaluated a non-probabilistic consecutive sample of 38 children referred to a sleep laboratory for suspicion of OSAHS between June of 2003 and December of 2004. The patients were submitted to polysomnography and to a pre-sleep questionnaire, developed by the authors, based on other questionnaires reported in the literature.(8,9) The questionnaire was applied to the patients and their companions. It was composed of questions designed to collect various types of data: demographic and anthropometric characteristics (age, weight and height); sleep aspects (snoring, bruxism, observed apnea, excessive movement during sleep and awakenings); daytime symptoms (daytime sleepiness, difficulty in waking up, headaches upon waking, hyperactivity, difficulty in learning at school and aggressiveness); sports (type, frequency and time of day); and medical records/comorbidities (tonsils and adenoids hypertrophy, nasal obstruction, preterm delivery, asthma, sinusitis, gastroesophageal reflux disease, sickle cell anemia, heart/lung disease, epilepsy, isolated convulsive seizures, food allergy, stunted growth/development, previous surgery, use of medications and other diseases). The evaluated children were divided into two groups according to age bracket: up to six years of age (the period that coincides with the peak of lymphoid hypertrophy); and over six years of age.
The polysomnographic findings were obtained using a Sonolab 620 (Medtron, São Paulo, Brazil), and the following variables were analyzed: electroencephalography, right and left electrooculogram; electromyography of the chin, nasal and oral flux (using a thermistor and nasal cannula), thoracic and abdominal belts, electrocardiogram, arterial oxygen saturation (using a pulse oximeter), body position (using a body position sensor), leg movement (using electrodes on the legs), intensity of the snoring (using a microphone).
Sleep was staged using the classification established by Rechtschaffen and Kales.(10) The micro-arousals were detected according to the criteria published by Bonnet et al.(11) In accordance with the criteria of the American Thoracic Society, obstructive apnea was defined as complete cessation of the nasal and mouth air flow of any duration, followed by the thoracic and abdominal movement, thus excluding the cases of central apnea. Obstructive hypopnea was defined as a decrease of at least 50% of the baseline flow associated with the desaturation of 4% or more and/or micro-arousals.(12) The apnea-hypopnea index (AHI) was calculated based on the number of obstructive apneas and hypopnea events occurring during one hour of sleep. The adopted classification of the severity of OSAHS, following the parameters for the pediatric age bracket, was normal with an AHI < 1; mild with an AHI between 1 and 5; moderate when the AHI is between 5 and 10 and serious when the AHI is >10.(13-15)
The parents or legal guardians of all children included in the study agreed to participate and gave written informed consent. The statistical analysis was carried out using the Statistical Package for the Social Sciences, version 10.0 (SPSS Inc., Chicago, IL, USA). The chi-square test was used in order to compare categorical variables. Student's t-test or Mann-Whitney test was used to compare the means, according to the distribution of the variable in question. The level of significance adopted was 5%.
ResultsThirty eight children were evaluated. The mean age was 8.4 ± 3.99 years (range, 2-15 years), and 50% of the children were male. There were 3 children (7.9%) who were non-apneic, 16 (42.1%) who presented mild obstructive sleep disorder, 11 (28.9%) who presented moderate obstructive sleep disorder and 8 (21.1%) who presented severe obstructive sleep disorder. The mean AHI was 9.59 ± 56.2 (range, 1.2-56.2).
Among the children with obstructive sleep disorder, the symptoms most often reported were snoring and nasal obstruction, which occurred in 75.8 and 73.3%, respectively. Complaints of restless legs during sleep were found in 61.1 and 37.5% reported difficulty in falling sleep. Bruxism and excessive sleepiness occurred in 31.3 and 29% of the cases. Awakening during the night due to a sensation of suffocating was reported by 25% of the companions of the studied children. Headaches upon waking were present in 6.7% of the children in the study, whereas reflux disease was present in only 3.1% (Figure 1).

All children who presented severe obstructive sleep disorder complained of snoring and bruxism; the other two most frequently observed symptoms were nasal obstruction and restless legs during sleep, both present in 75% of the examined patients with severe disorder.
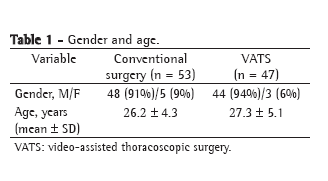
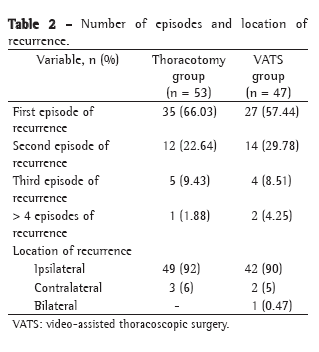
The polysomnographic parameters of the children included by OSAHS severity and by age bracket are described in Tables 1 and 2, respectively.
When analyzing the influence of age on the severity of OSAHS, we observed that all of the severe cases occurred in children up to six years of age (preschoolers - Figure 2). In relation to the symptoms, all of the children up to six years of age presented snoring, compared to 55% of the children over six years of age, this difference being statistically significant (p = 0.004). There were no differences between the two groups in relation to the other symptoms.
 Discussion
DiscussionThe present study describes children who were referred to a sleep laboratory for suspicion of having OSAHS. Most of the children presented polysomnographic alterations consistent with this diagnosis, the most severe cases occurring most often in children up to six years of age.
Anamnesis is a fundamental step for the diagnosis of obstructive sleep disorders in children. However, previous studies have shown weak correlations between clinical symptoms and polysomnographic findings. In 1995, Carroll et al. compared answers to a questionnaire referring to clinical symptoms of OSAHS and polysomnographic findings in children with adenotonsillar hypertrophy. A poor correlation was found between symptoms and polysomnography.(16) Questionnaires that collect clinical history or physical examination data do not have good predictive value to the diagnosis of OSAHS in children.(17) Their sensitivity and specificity are only 35 and 39%, respectively.(18) This is due, principally, to the fact that such questionnaires depend on the reports of companions, who often do not know exactly which symptoms are presented during sleep.(17)
In our study, snoring was the symptom most frequently found in children and adolescents with OSAHS. This result is in accordance with the literature, which indicates snoring as the most important clinical predictor of a diagnosis of OSAHS in children, with good sensitivity (91%) and reasonable specificity (75%).(19-21) Nasal obstruction and restless legs during sleep were other symptoms that presented a high prevalence in our study, although not correlating significantly with OSAHS in other studies.(19) Daytime sleepiness, a symptom frequently observed in adults with OSAHS, is not one of the principal symptoms in children,(22) being present in only 29% of the cases in our sample. In other studies, daytime sleepiness has been found in up to 19% of non-snoring children and up to 30% of habitually snoring children.(20) Other symptoms that are currently considered important to the diagnosis of OSAHS in children are restless sleep, night sweats and nocturnal enuresis.(1)
Since clinical history is not effective in differentiating between, for example, OSAHS and primary snoring, the gold standard for the diagnosis is polysomnography, which must be carried out at a sleep laboratory during an entire night.(23) The high cost and complexity of the examination make its routine use difficult, since it is available in few places. In addition, education regarding sleep-disordered breathing in children is still unsatisfactory, so that the diagnostic method of choice remains unknown to many pediatricians, who typically diagnose OSAHS based on their clinical experience.(24)
The fact that the most severe cases of OSAHS occur in preschoolers (under six years of age) is probably best explained by the higher occurrence of adenoid and tonsil hypertrophy (the principal causal factor of the obstructive sleep apnea syndrome in children) in this population, although other factors, such as pharyngeal muscle tone and genetic influences, can play a role. Marcus reported that the pathogenesis of the OSAHS is due to the combination of structural factors (adenoid and tonsil hypertrophy); craniofacial anomalies and neurological factors.(22) In each case one of these factors predominates. Valera et al. showed a greater tendency of OSAHS in preschoolers with the same degree of adenotonsillar obstruction, suggesting the influence of neurological and muscle maturation, as related by Ward and Marcus.(6,16)
Stunted growth (weight and height) is most commonly observed in children with OSAHS, who experience an increase in the rate of growth after undergoing tonsillectomy.(25) Decreased production of the growth hormone during fragmented sleep and increased respiratory effort can contribute to the deficit in the growth of these children,(5) as well as to the cardiovascular alterations including pulmonary hypertension and right ventricle dysfunction, which can be potentially avoided by surgically removing the adenoid and tonsillar tissue. The true prevalence of these alterations is as yet unknown. Systemic arterial hypertension, commonly found in adults with OSAHS, has also been described in children.(26)
In children, OSAHS can have a negative impact on academic performance. The incidence to OSAHS is six to nine times greater in children with learning problems at school than in the general pediatric population.(27)
In a study by Ali et al., who evaluated 50 children with polysomnography-confirmed OSAHS, 84% presented excessive daytime sleepiness, 76% had a behavior disorder, 42% were hyperactive, and 16% presented substandard academic performance.(28) A significant improvement in academic performance can be observed a year after the surgical removal of the hypertrophied adenoid and tonsillar tissue.(27) However, to what extent this process is totally reversible remains uncertain. Goza et al. suggest that a decrease in academic performance in the long term can represent a residual and irreparable cognitive deficit in children who had OSAHS during a critical phase of the development of abilities and aptitudes, even years after the resolution of the problem.(29)
This study is relevant because it emphasizes the importance of OSAHS in the pediatric population, identifies the symptoms most frequently associated with this pathology in Brazil and the factors associated with greater severity of the disease. Future studies will be able to provide a better definition of the specificity of these symptoms for the diagnosis of OSAHS. However, the results of the present study must be considered in the context of some limitations. The principal limitations are the relatively small number of patients and the absence of a control group composed of children without OSAHS. There is still controversy in the literature in relation to the types of respiratory events that should be used as criteria for the diagnosis of OSAHS in children and adolescents. While the use of the AHI is well-accepted for the classification of OSAHS in adults, some authors believe that, in pediatric patients, it should be based only on the obstructive apnea index, since there is no consensus in relation to the definition of hypopnea.(30) In the present study we chose to use the AHI for the diagnosis and classification of OSAHS in children, since this is the procedure adopted by the authors in their clinical practice and is in accordance with many recently published studies on the theme.(13-15)
We concluded that the symptoms most frequently observed in children and adolescents with OSAHS in this study were snoring and chronic nasal obstruction. In addition, the most severe cases of OSAHS occur in children under six years of age, which coincides with the peak of the lymphoid growth in this age bracket. Therefore, the evaluation of the sleep disorders in children who presented symptoms such as snoring and nasal obstruction is necessary, due to the negative impact that these alterations can have on physiological and neurocognitive development Pediatricians must attempt to recognize suspected cases and refer them to specialized clinics. These clinics, in turn, must evaluate and counsel the patient in order to achieve early diagnosis and treatment, avoiding the occurrence of the severe complications related to this syndrome.
References 1. Schechter MS; Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome. Technical report: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics. 2002;109(4):e69.
2. Osler W. Chronic tonsillitis. In: Osler W, editor. The principles and practice of medicine. New York: Appleton and Co.; 1892. p. 335-9.
3. Valera FC, Demarco RC, Anselmo-Lima WT. Síndrome da Apnéia e da Hipopnéia Obstrutivas do Sono (SAHOS) em crianças. Rev Bras Otorrionolatingol. 2004;70(2):232-7.
4. Weissbluth M, Davis AT, Poncher J, Reiff J. Signs of airway obstruction during sleep and behavioral, developmental, and academic problems. J Dev Behav Pediatr. 1983;4(2):119-21.
5. Chan J, Edman JC, Koltai PJ. Obstructive sleep apnea in children. Am Fam Physician. 2004;69(5):1147-54.
6. Ward SL, Marcus CL. Obstructive sleep apnea in infants and young children. J Clin Neurophysiol. 1996;13(3):198-207.
7. Suen JS, Arnold JE, Brooks LJ. Adenotonsillectomy for treatment of obstructive sleep apnea in children. Arch Otolaryngol Head Neck Surg. 1995;121(5):525-30.
8. Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP. Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med. 1999;131(7):485-91.
9. Brouilette R, Hanson D, David R, Klemka L, Szatkowski A, Fernbach S, et al. A diagnostic approach to suspected obstructive sleep apnea in children. J Pediatr. 1984;105(1):10-4.
10. Kales A, Rechtschaffen A, editors. A manual of standardized terminology, techniques and scoring system for sleep stages of human subjects. National Institutes of Health publication, no. 204. Bethesda, Md: U. S. National Institute of Neurological Diseases and Blindness, Neurological Information Network; 1968.
11. EEG arousals: scoring rules and examples: a preliminary report from the Sleep Disorders Atlas Task Force of the American Sleep Disorders Association. Sleep. 1992;15(2):173-84.
12. Standards and indications for cardiopulmonary sleep studies in children. American Thoracic Society. Am J Respir Crit Care Med. 1996;153(2):866-78.
13. Harvey JM, O'Callaghan MJ, Wales PD, Harris MA, Masters IB. Aetiological factors and development in subjects with obstructive sleep apnoea. J Paediatr Child Health. 1999;35(2):140-4.
14. Balbani AP, Weber SA, Montovani JC. Update in obstructive sleep apnea syndrome in children. Rev Bras Otorrinolaringol (Engl Ed). 2005;71(1):74-80.
15. Ramos RT, da Cunha Daltro CH, Gregório PB, de Freitas Souza LS, de Andrade NA, de Souza Andrade Filho A, et al. OSAS in children: clinical and polysomnographic respiratory profile. Rev Bras Otorrinolaringol (Engl Ed). 2006;72(3):355-61.
16. Valera FC, Avelino MA, Pettermann MB, Fujita R, Pignatari SS, Moreira GA, et al. OSAS in children: correlation between endoscopic and polysomnographic findings. Otolaryngol Head Neck Surg. 2005;132(2):268-72.
17. Carroll JL, McColley SA, Marcus CL, Curtis S, Loughlin GM. Inability of clinical history to distinguish primary snoring from obstructive sleep apnea syndrome in children. Chest. 1995;108(3):610-8.
18. Brouilette R, Hanson D, David R, Klemka L, Szatkowski A, Fernbach S, et al. A diagnostic approach to suspected obstructive sleep apnea in children. J Pediatr. 1984;105(1):10-4.
19. Chau KW, Ng DK, Kwok CK, Chow PY, Ho JC. Clinical risk factors for obstructive sleep apnoea in children. Singapore Med J. 2003;44(11):570-3.
20. Kaditis AG, Finder J, Alexopoulos EI, Starantzis K, Tanou K, Gampeta S, et al. Sleep-disordered breathing in 3,680 Greek children. Pediatr Pulmonol. 2004;37(6):499-509.
21. Ersu R, Arman AR, Save D, Karadag B, Karakoc F, Berkem M, et al. Prevalence of snoring and symptoms of sleep-disordered breathing in primary school children in istanbul. Chest. 2004;126(1):19-24.
22. Marcus CL. Sleep-disordered breathing in children. Am J Respir Crit Care Med. 2001;164(1):16-30.
23. Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome. American Academy of Pediatrics. Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics. 2002;109(4):704-12.
24. Balbani AP, Weber SA, Montovani JC, Carvalho LR. [Pediatricians and sleep-disordered breathing in the child][Article in Portuguese]. Rev Assoc Med Bras. 2005;51(2):80-6.
25. Lind MG, Lundell BP. Tonsillar hyperplasia in children. A cause of obstructive sleep apneas, CO2 retention, and retarded growth. Arch Otolaryngol. 1982;108(10):650-4.
26. Marcus CL, Greene MG, Carroll JL. Blood pressure in children with obstructive sleep apnea. Am J Respir Crit Care Med. 1998;157(4 Pt 1):1098-103.
27. Gozal D. Sleep-disordered breathing and school performance in children. Pediatrics. 1998;102(3 Pt 1):616-20.
28. Ali NJ, Pitson D, Stradling JR. Natural history of snoring and related behaviour problems between the ages of 4 and 7 years. Arch Dis Child. 1994;71(1):74-6.
29. Gozal D, Pope DW Jr. Snoring during early childhood and academic performance at ages thirteen to fourteen years. Pediatrics. 2001;107(6):1394-9.
30. Guilleminault C, Lee JH, Chan A. Pediatric obstructive sleep apnea syndrome. Arch Pediatr Adolesc Med. 2005;159(8):775-85.
____________________________________________________________________________________________________________________
Study carried out at the Sleep Laboratory of the Cardiopulmonary Institute, Salvador, Brazil.
1. Pulmonologist. Cardiopulmonary Institute, Salvador, Brazil
2. Resident Physician. Universidade Federal de São Paulo - UNIFESP, Federal University of São Paulo - Hospital São Paulo, São Paulo, Brazil.
3. Medical Student. Universidade Federal da Bahia - UFBA, Federal University of Bahia - School of Medicine, Salvador, Brazil
4. Medical Student. Escola Bahiana de Medicina e Saúde Pública - EBMSP, Bahia School of Medicine and Public Health - Salvador, Brazil.
5. Graduate Student in Medicine and Human Health in the Fundação Baiana para Desenvolvimento das Ciências - FBDC, Bahia Foundation for Science Development - Salvador, Brazil.
6. Head of the Sleep Laboratory of the Cardiopulmonary Institute, Salvador, Brazil.
Correspondence to: Paloma Baiardi Gregório. Rua Macaúbas, 428, apto. 304, CEP 41940250, Rio Vermelho, Salvador, BA, Brazil.
Tel 55 71 3346-1466 / 9135-9101; Fax 55 71 3245-0858. E-mail: palomabg@ig.com.br
Submitted: 31 January 2007. Accepted, after review: 21 August 2007.







