ABSTRACT
Objective: To evaluate the use of the forced expiratory volume in one second/forced expiratory volume in six seconds (FEV1/FEV6) ratio
as an alternative to the FEV1/forced vital capacity (FVC) ratio in the detection of mild airway obstruction. Methods: Reference equations
for the Brazilian population in 2006 were used in order to determine the lower limits of normality for the FEV1/FEV6 and FEV1/FVC ratios.
The spirometry findings of 155 patients from 20 to 84 years of age were analyzed. All of the patients presented the following: a < 15%
difference between predicted and observed FEV1/FVC ratio; an FEV1 ≥ 60% of predicted; and an exhalation time of at least 6 s. The
Brazilian Thoracic Society criteria for acceptability and reproducibility in spirometry were met. Results: Mean values (± SD) for FEV1/FEV6
and FEV1/FVC were 73 ± 4% and 75 ± 3%, respectively. Using the FEV1/FVC ratio, we identified airflow obstruction in 61 patients, compared
with only 46 patients when we used the FEV1/FEV6 ratio, showing a sensitivity of 75% (p < 0.001). Conclusions: The FEV1/FEV6 ratio has
poor sensitivity and should not be used to replace the FEV1/FVC ratio in the diagnosis of mild airway obstruction.
Keywords:
Forced expiratory volume; Vital capacity; Airway obstruction; Spirometry; Respiratory function tests.
RESUMO
Objetivo: Avaliar a utilidade da relação volume expiratório forçado no primeiro segundo/volume expiratório forçado nos primeiros seis
segundos (VEF1/VEF6) na detecção de obstrução leve ao fluxo aéreo como alternativa à relação VEF1/capacidade vital forçada (CVF).
Métodos: As equações sugeridas para a população brasileira em 2006 foram utilizadas para determinar os limites inferiores normais para as
relações entre VEF1/VEF6 e VEF1/CVF. Foram avaliadas as espirometrias de 155 pacientes com diferença entre a relação VEF1/CVF previstaobservada
abaixo de 15% e VEF1 ≥ 60% do previsto, com idades entre 20 e 84 anos e com tempo expiratório de 6 s no mínimo. Os critérios
de aceitabilidade e reprodutibilidade para a espirometria sugeridos pela Sociedade Brasileira de Pneumologia e Tisiologia foram preenchidos.
Resultados: Os valores médios (± dp) para VEF1/CVF e VEF1/VEF6 foram, respectivamente, 73 ± 4% e 75 ± 3%. A obstrução ao fluxo aéreo
foi detectada pela relação VEF1/CVF em 61 pacientes, mas foi detectada pela relação VEF1/VEF6 em apenas 46 deles, mostrando uma sensibilidade
de 75% (p < 0,001). Conclusões: A relação VEF1/VEF6 tem sensibilidade insuficiente para substituir a relação VEF1/CVF no diagnóstico
de obstrução leve ao fluxo aéreo.
Palavras-chave:
Volume expiratório forçado; Capacidade vital; Obstrução das vias respiratórias; Espirometria; Testes de função pulmonar.
IntroductionSpirometry is a noninvasive affordable test with many clinical applications and allows the diagnosis of numerous lung diseases.(1)
Obstructive lung disease (OLD), principally observed in individuals with asthma and chronic obstructive pulmonary disease (COPD), is characterized by reduced expiratory flow in relation to expiratory lung volume. The classical parameter used to characterize lung diseases as obstructive is the reduction in the ratio between forced expiratory volume in one second and forced vital capacity (FEV1/FVC ratio). The FVC maneuver is a test that requires effort and collaboration from the patient. For the test to meet the acceptability and reproducibility criteria, patients must empty their lungs completely in at least three maneuvers. Each of these maneuvers can last up to 20 s and are exhausting for debilitated patients, older patients and patients with advanced lung disease. In normal individuals, the duration of the FVC maneuver increases with age.(1,2)
In recent years, the FEV1/FEV in six seconds (FEV1/FEV6) ratio was proposed as a parameter for use in the diagnosis of OLD. Using this ratio would have the following advantages: greater convenience for the patient during the performance of the test, since it would last only 6 s; reduced risk of syncope (albeit rare); greater ease in meeting acceptability and reproducibility criteria; and, finally, the ability to perform tests rapidly using portable spirometers, allowing the early en masse diagnosis of OLD.(3-10) Predicted values for this ratio have been recently derived for the Brazilian population.(11)
The positive impact of early diagnosis in patients with OLD would principally affect patients who present subtle symptoms and minimal alterations on pulmonary function tests. Many studies have assessed the sensitivity of the FEV1/FEV6 ratio in the diagnosis of airway obstruction.
However, young patients and patients with moderate or pronounced obstruction have been included in such studies, inflating the sensitivity of the test.(5,7,9,10) Reduced end-expiratory flows and prolonged expiratory time, which can exceed 6 s, occur in the initial stage of airway obstruction. The FEV1/FEV6 ratio can therefore lose sensitivity in early diagnosis, especially in aging patients, in whom the time required to complete the FVC maneuver increases progressively.
The objective of the present study was to assess the sensitivity of the FEV1/FEV6 ratio in the diagnosis of mild airflow limitation.
MethodsWe evaluated 155 consecutive Caucasian patients who underwent spirometry at the pulmonary function laboratories of the São Paulo Hospital for State Civil Servants and Brazil Diagnostic Center. Technicians certified in pulmonary function by the Brazilian Thoracic Society (BTS) carried out the tests using two spirometers (SensorMedics, Yorba Linda, CA, USA). The following inclusion criteria were applied: presenting < 15% difference between the predicted and observed FEV1/FVC ratio; having an FEV1 ≥ 60% of predicted; and meeting the BTS criteria for acceptability and reproducibility (including exhalation time of at least 6 s). The reference values used were predicted values recently proposed for the Brazilian population.(11) For all of the cases included, age and height were within the range of observed values for each gender in the sample from which reference equations were derived. Ratio values derived from this study are shown in Chart 1.

The sensitivity of the FEV1/FEV6 ratio was calculated based on data published in four studies, considering only patients with mild airway obstruction.(5,7,8,10) The mean sensitivity in those studies was 76% (24% false-negative results). Considering this value for the number of false-negatives using the FEV1/FEV6 ratio and a 15% lower limit of 95% CI (a value considered high and unacceptable), it would be necessary to analyze at least 90 spirometry tests in order to confirm these data.(12)
This was a retrospective study using routine functional tests requested by attending physicians or periodic health tests, performed under the doctor-patient privilege. The study was approved with no restrictions by the Ethics Committee of the Institute for the Medical Treatment of Civil Servants, protocol no. 031/07.
Airway obstruction was characterized by FEV1/FVC ratio values below the 5th percentile of predicted. Values for FEV1/FVC and FEV1/FEV6 ratios classified as normal or reduced were compared using the chi-square test. In the statistical analysis, we used was the Statistical Package for Social Sciences, version 10 (SPSS, Chicago, IL, USA).(13)
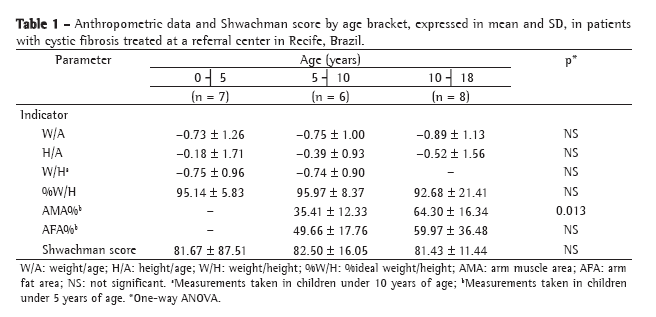
ResultsThe general characteristics of the sample are described in Table 1.
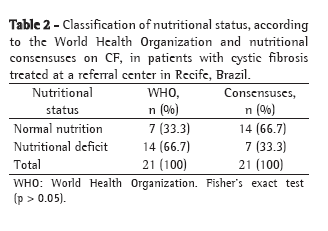
The FEV1/FVC ratio identified airway obstruction in 61 patients, compared with only 46 patients for the FEV1/FEV6 ratio (p < 0.001). There was one false-positive result. Sensitivity of the FEV1/FEV6 ratio for the detection of mild airway obstruction was therefore 75% (p < 0.0001) and specificity was 99%, as can be seen in Table 2. The 95% CI calculated for this sample was 19 to 31%.
 Discussion
DiscussionIn the present study, using the FEV1/FEV6 ratio in the diagnosis of mild airway obstruction resulted in a great number of false-negatives.
The lower limit of the FEV1/FVC ratio is established by subtracting 7.6 and 8.5 from predicted values in males and females, respectively, in the Brazilian population.(11) In the present study, sample selection was restricted to cases with a < 15% difference between predicted and observed FEV1/FVC ratio and with a FEV1 ≥ 60%. This was done in order to include only patients presenting normal spirometry findings or spirometry findings of mild airway obstruction.
One study assessed 337 spirometry findings of normal individuals and patients with OLD or restrictive lung disease.(7) In that study, the sensitivity of the FEV1/FEV6 ratio was found to be 95%. Only 41 patients (12.1%) presented mild OLD. All cases with discordant FEV1/FEV6 and FEV1/FVC ratios presented FEV1/FVC ratio values near the lower limit of normality, with a maximum difference of four percentage points. When the group of patients with mild obstruction was analyzed independently, the sensitivity of the FEV1/FEV6 ratio in the diagnosis of mild OLD dropped to 73%.
Another study(5) assessed the spirometry findings for 11,676 patients aged 20-80 years. The authors observed that the sensitivity of the FEV1/FEV6 ratio, in comparison with the FEV1/FVC ratio, was 94%. In that sample, 13.3% of the patients had mild OLD. Similarly to the findings of the previously cited study, 100% of discordant patients were near the lower limit of normality. When the group of patients with mild obstruction was analyzed independently, the sensitivity of the FEV1/FEV6 ratio for the diagnosis of mild OLD was 82%.
Another study(9) assessed the spirometry findings for 1,139 workers aged 18-71 years. The study showed 92% sensitivity for the FEV1/FEV6 ratio. This sample was principally composed of patients with normal spirometry results: only 14.4% presented obstruction (the severity of the obstruction was not classified). In addition, the mean age of the patients studied was 37 years, which inflates the sensitivity of the FEV1/FEV6 ratio.
One group of authors(10) studied 1,926 spirometry tests, evaluating the sensitivity of the FEV1/FEV6 ratio in different ethnic groups and with varying degrees of airway obstruction. The overall sensitivity was 85.6%. The sensitivity of the ratio ranged from 74% (among patients with mild obstruction) to 100% (among patients with pronounced obstruction).
The results obtained in the present study are in agreement with the data found by the abovementioned authors(5,7,9,10) and clearly show that the FEV1/FEV6 ratio has poor sensitivity for the detection of mild airway
obstruction.
Other authors,(14) based on a study of individuals over the age of 60, suggested that the 73% value for the FEV1/FEV6 ratio could be used in place of the fixed value of 70% for the FEV1/FVC ratio proposed by the Global Initiative for Chronic Obstructive Lung Disease (GOLD) consensus(15) for characterizing airway obstruction. The limitations of the use of a fixed FEV1/FVC ratio value to characterize obstruction are widely recognized.(16-18) The FEV1/FVC ratio drops with age.(11) In the Brazilian population, the lower limit of 70% is reached at the mean age of 65 years for males and 70 years for females.(11) Smokers who are sensitive to the effects of tobacco will present reduced values for the FEV1/FVC ratio at approximately 45 years of age. At this age, the lower limit of the predicted value is approximately 75%. Based on these data, the frequency of airway obstruction detection will be insufficient in the age bracket in which COPD is incipient, whereas it will be exacerbated in older individuals.(18)
Although all smokers should be encouraged to stop smoking, the detection of airway obstruction can result in greater cessation, as has been demonstrated in some studies.(19)
After the present study had been concluded, a national field study compared the sensitivity of the FEV1/FEV6 ratio with that of the FEV1/FVC ratio.(20) In that study, only two curves were considered acceptable, and no reference was made to the race of the individuals tested. Obstruction was considered present when the FEV1/FVC ratio was <70%. Regarding the FEV1/FEV6 ratio, the individual lower limits suggested by Hankinson were used, regardless of race (there are values for Caucasians, Mexican-Americans and for blacks, derived from the North-American population).
These data might represent an underestimation of the sensitivity of the FEV1/FVC ratio and an overestimation of the sensitivity of the FEV1/FEV6 ratio.
In a Brazilian sample of individuals without cardiorespiratory disease,(11) the mean expiratory time was 7.07 ± 1.56 s in 270 males aged 26-86 years, compared with 6.13 ± 1.35 s among 373 females aged 20-85 years. Expiratory time was typically below 6 s in males under the age of 45 years and in females under 50 years. However, expiratory times longer than 6 s are often observed in lower age brackets.(11)
In the online version of the GOLD consensus, it was recently stated that the use of a fixed cut-off point of 70% can result in false-positive results in older individuals. However, in the same document, it is clear that the fixed FEV1/FVC ratio < 70% continues to be the recommended cut-off point for characterizing airway obstruction.(21) In addition, the GOLD consensus recommends that this value be obtained after the use of a bronchodilator, a parameter for which reference values are unavailable.
Incipient obstruction in diffuse distal obstructive diseases such as COPD and asthma is a result of slow end-expiratory flows with prolonged expiratory time. From a pathophysiological standpoint, it is difficult to understand how the FEV1/FEV6 ratio can be below the lower limit of predicted in a certain number of cases in which the FEV1/FVC ratio remains normal.(5,7) In our study, there was only one case in which there was an isolated reduction in the FEV1/FEV6 ratio.
All of the previously mentioned studies used the Hankinson equation as a reference value of normality.(3) The reference values used in the present study were those recently proposed for the Brazilian population.(11) They differ significantly from the values proposed by Hankinson.(3) The predicted values for FEV1/FVC and FEV1/FEV6 ratios are lower in individuals of shorter stature, due to the effect of greater dynamic compression resulting from greater muscle strength.(11) Not correcting values for height results in overestimated frequency of airway obstruction in taller individuals.(11) In the equations proposed by Hankinson, the regressions are adjusted only for age.
From the epidemiological point of view and considering the evolution of the disease, early detection of COPD is important. However, it is made difficult by the use of the FEV1/FEV6 ratio.
In conclusion, the FEV1/FEV6 ratio has poor sensitivity and should not be used as a substitute for the FEV1/FVC ratio in the diagnosis of mild airway obstruction in Brazilian Caucasians.
References 1. Pereira CA. Espirometria. J. Pneumol. 2002;28(supl.3):1-82.
2. Ferguson GT, Enright PL, Buist AS, Higgins MW. Office spirometry for lung health assessment in adults: A consensus statement from the National Lung Health Education Program. Chest. 2000;117(4):1146-61.
3. Hankinson JL, Odencrantz JR, Fedan KB. Spirometric reference values from a sample of the general U.S. population. Am J Respir Crit Care Med. 1999;159(1):179-87.
4. Hankinson JL, Crapo RO, Jensen RL. Spirometric reference values for the 6-s FVC maneuver. Chest. 2003;124(5):1805-11.
5. Vandevoorde J, Verbanck S, Schuermans D, Kartounian J, Vincken W. Obstructive and restrictive spirometric patterns: fixed cut-offs for FEV1/FEV6 and FEV6. Eur Respir J. 2006;27(2):378-83.
6. Enright RL, Connett JE, Bailey WC. The FEV1/FEV6 predicts lung function decline in adult smokers. Respir Med. 2002;96(6):444-9.
7. Swanney MP, Jensen RL, Crichton DA, Beckert LE, Cardno LA, Crapo RO. FEV(6) is an acceptable surrogate for FVC in the spirometric diagnosis of airway obstruction and restriction. Am J Respir Crit Care Med. 2000;162(3 Pt 1):917-9.
8. Vandevoorde J, Verbanck S, Schuermans D, Kartounian J, Vincken W. FEV1/FEV6 and FEV6 as an alternative for FEV1/FVC and FVC in the spirometric detection of airway obstruction and restriction. Chest. 2005;127(5):1560-4.
9. Akpinar-Elci M, Fedan KB, Enright PL. FEV6 as a surrogate for FVC in detecting airways obstruction and restriction in the workplace. Eur Respir J. 2006;27(2):374-7.
10. Fukunaga M, Kim EJ, Sundaram SC, Sullivan J, Friedmann P, Salzman SH. Forced expiratory volume in 1 second/forced expiratory volume in 6 seconds (FEV1/FEV6) is a suboptimal surrogate for FEV1/Forced vital capacity (FEV1/FVC) in the spirometric diagnosis of airflow obstruction in a diverse urban population. Chest. 2005;128(4):172S.
11. Pereira CA; Sato T; Rodrigues SC. New reference values for forced spirometry in white adults in Brazil. J Bras Pneumol. 2007;33(4):397-406.
12. Ingelfinger JA, Mosteller F. Thibodeau LA, Ware JH. Assessing treatment efficacy by analyzing counts. In: Ingelfinger JA, Mosteller F. Thibodeau LA, Ware JH, editors. Biostatistics in clinical medicine. 3rd Ed. New York: McGraw-Hill; 1994. p. 132-54.
13. SPSS - Statistical Package for the Social Sciences [homepage on the Internet]. Chicago: SPSS Inc. [cited 2007 July 21]. Available from: http://www.spss.com
14. Melbye H, Medbø A, Crockett A. The FEV1/FEV6 ratio is a good substitute for the FEV1/FVC ratio in the elderly. Prim Care Respir J. 2006;15(5):294-8.
15. Pauwels RA, Buist AS, Calverley PM, Jenkins CR, Hurd SS; GOLD Scientific Committee. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. NHLBI/WHO Global Initiative for Chronic Obstructive Lung Disease (GOLD) Workshop summary. Am J Respir Crit Care Med. 2001;163(5):1256-76.
16. Hardie JA, Buist AS, Vollmer WM, Ellingsen I, Bakke PS, Mørkve O. Risk of over-diagnosis of COPD in asymptomatic elderly never-smokers. Eur Respir J. 2002;20(5):1117-22.
17. Roberts SD, Farber MO, Knox KS, Phillips GS, Bhatt NY, Mastronarde JG, et al. FEV1/FVC ratio of 70% misclassifies patients with obstruction at the extremes of age. Chest. 2006;130(1):200-6.
18. Hansen JE, Sun XG, Wasserman K. Spirometric criteria for airway obstruction: Use percentage of FEV1/FVC ratio below the fifth percentile, not < 70%. Chest. 2007;131(2):349-55.
19. Bednarek M, Gorecka D, Wielgomas J, Czajkowska-Malinowska M, Regula J, Mieszko-Filipczyk G, et al. Smokers with airway obstruction are more likely to quit smoking. Thorax. 2006;61(10):869-73.
20. Lundgren FL, Cabral MM, Clímaco DC, Macedo LG, Coelho MA, Dias AL. Determination of the efficacy of FEV6 as a surrogate for FVC in the diagnostic screening for chronic obstructive pulmonary disease through the comparison of FEV1/FVC and FEV1/FEV6 ratios. J Bras Pneumol. 2007; 33(2):148-51.
21. GOLD Global Initiative for Chronic Obstructive Lung Disease [homepage on the Internet]. [updated 2006 Nov; cited 2007 July 21]. Available from: www.goldcopd.com
____________________________________________________________________________________________________________________
Study carried out in the Pulmonary Function Laboratory of the Hospital do Servidor Público Estadual de São Paulo - HSPE-SP, São Paulo Hospital for State Civil Servants - São Paulo, Brazil.
1. Graduate Student in Pulmonology. Hospital do Servidor Público Estadual de São Paulo - HSPE-SP, São Paulo Hospital for State Civil Servants - São Paulo, Brazil.
2. Director of the Pulmonary Function Laboratory at the Hospital do Servidor Público Estadual de São Paulo - HSPE-SP, São Paulo Hospital for State Civil Servants - São Paulo, Brazil.
3. Head of the Pulmonology Department. Hospital do Servidor Público Estadual de São Paulo - HSPE-SP, São Paulo Hospital for State Civil Servants - São Paulo, Brazil.
Correspondence to: André Luis Pinto Soares. Rua Pedro de Toledo, 1800, Vila Clementino, CEP 04039-901, São Paulo, SP, Brasil.
Tel/Fax 55 11 5574-6603. E-mail:drandrepinto@globo.com
Submitted: 21 July 2007. Accepted, after review: 26 September 2007.






